By: Dr. Elizabeth Eggert
Whether or not you need dentures depends on your unique oral situation. We are lucky to be in an age where very few people are unable to keep their natural teeth for a lifetime. However, even with a lifetime of quality care, it is possible to end up in a situation where dentures make the most sense as a tooth replacement option.
Let’s discuss what dentures are, how they work, and when it’s time to come in for an appointment to see if dentures are right for you.
What Are Dentures and How Do They Work?
Traditional dentures are a set of false teeth that can replace all upper or lower teeth. They attach to a gum-colored, acrylic base that sits directly over your gum tissue. These dentures are removable, and sometimes need adhesive strips or paste to help them stay in.
Not only can dentures improve the appearance of the smile, but they also support the structure of the cheeks and lips. Dentures are often used as the solution for advanced cases of:
- Tooth loss
- Tooth decay
- Tooth pain
- Tooth injury
- Tooth and gum infection
While many patients report that dentures take time to get used to, dentures allow patients to look fairly normal when they smile, talk, and chew food, after an adjustment period, of course.
What are Dentures Made Of?
Dentures haven’t changed much in nearly 100 years, but in the last few years, innovations in 3D printing and design, have allowed for some new opportunities in denture design. If you don’t look too closely, they can look like real teeth. They have a gum-colored acrylic base and artificial teeth that can be made of porcelain, plastic, or hard resin.
Even though they’re false teeth, it’s important to care for your dentures as if they are real by brushing them daily to remove food particles and oral bacteria. Additionally, take care not to drop them or damage them, as they can become cracked.
It is also important to give your gum tissues a break and take your dentures out every night. Remove them before bed and place them in warm water or a denture cleaning solution like Efferdent.
2 Signs You Might Need Dentures
If you have any of the following dental conditions, it may be time to make an appointment with Dr. Eggert to see if dentures are right for you.
- Loose or missing teeth. Loose teeth can be a sign of periodontal (gum) disease and usually mean you are losing bone support for your teeth. At a certain point, if too much bone is lost, it becomes too difficult to treat the periodontal disease and Dr. Eggert may recommend that the most healthy treatment option is to remove the infected teeth and replace them with dentures.
- Chronic toothaches or non-restorable teeth. If you have chronic tooth infections and toothaches, it may be a sign that your teeth can no longer be restored or saved. The bacteria cannot be managed in any way other than the extraction of the teeth. Dr. Eggert will remove the infected teeth and dentures can replace what is lost.
Types of Dentures
Full Dentures
Full dentures replace all the teeth in your mouth and can either be conventional or immediate. Conventional dentures are made after your teeth have been removed, allowing the gums to heal. On the other hand, immediate dentures are made prior to surgery and can be placed immediately after tooth removal. (Immediate dentures will need many more adjustments as the gums heal and usually have to be remade within 1-2 years.)
Partial Dentures
A partial denture is a set of replacement teeth that attach to any remaining natural teeth. Typically, partial dentures use the same tooth and gum-colored acrylic of full dentures but are attached to a metal framework. Some all-plastic options are available today and these plastic frameworks have become much stronger than in the past and are typically thought to be more esthetic overall.
Implant Supported Denture
An implant supported denture, sits on the gums and is anchored into place with dental implants. Implant supported dentures can be designed to be removable or fixed in place. These dentures are much more secure than traditional dentures since the implants anchor very much like natural tooth roots. They can look very natural and can last a long time.
How Long Will It Take to Get My Dentures?
The process of getting dentures usually takes anywhere from a few weeks to many months. During your first appointment at Eggert Family Dentistry, Dr. Elizabeth Eggert or Dr. Jeff Eggert will need to determine which type of denture is right for you. Then, the process of fabricating dentures typically includes many impressions and try-in appointments to make sure the design will work best for you!
Think You Need Dentures? Call Us!
Getting older doesn’t have to mean losing your beautiful smile! If you think you might benefit from dentures, give Eggert Family Dentistry a call at 651.482.8412. Dr. Jeff Eggert or Dr. Elizabeth Eggert can address your concerns and discuss all the options available to you.

![Canker Sores vs. Cold Sores [and How to Treat Each!]](https://blog.eggertfamilydentistry.com/wp-content/uploads/2023/01/Cold-sore-vs-Canker-sore-825x506.png)


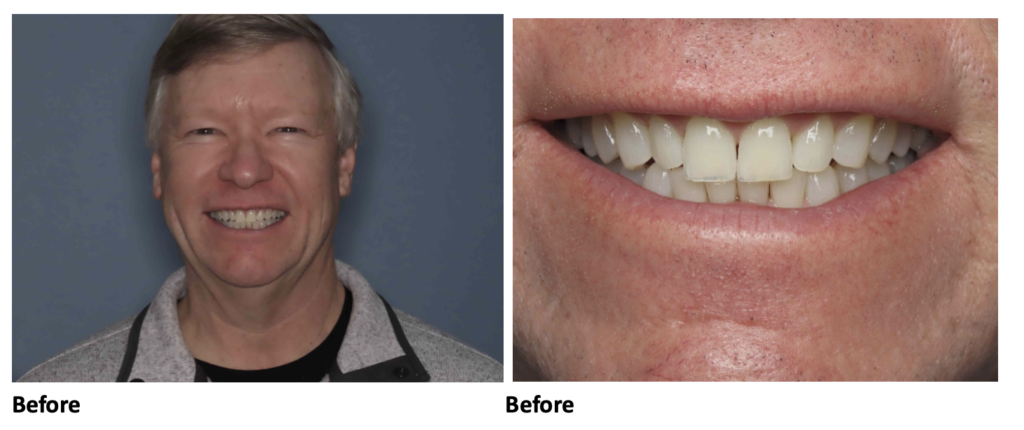
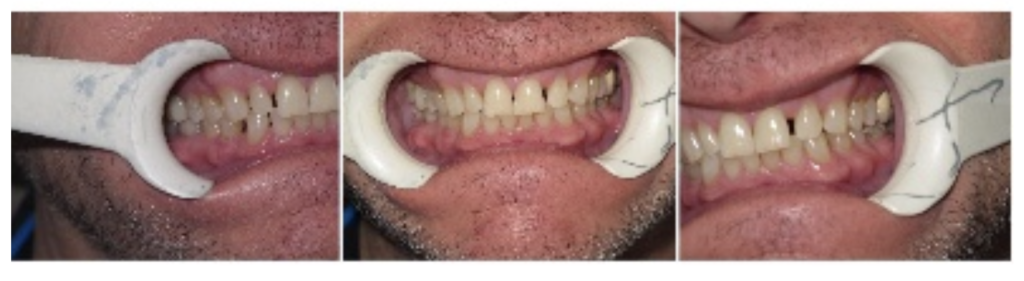 Pre-Initial Invisalign
Pre-Initial Invisalign