By: Dr. Elizabeth Eggert
April marked Oral Cancer Awareness Month, a crucial time dedicated to highlighting the importance of early detection and prevention of this often fatal disease. At Eggert Family Dentistry in North Oaks, MN, Dr. Elizabeth Eggert and Dr. Jeff Eggert took this opportunity to reinforce their unwavering commitment to your oral health. Throughout the month, they emphasized the importance of oral cancer screenings, which they incorporate into every recare check-up appointment.
Facts About Oral Cancer

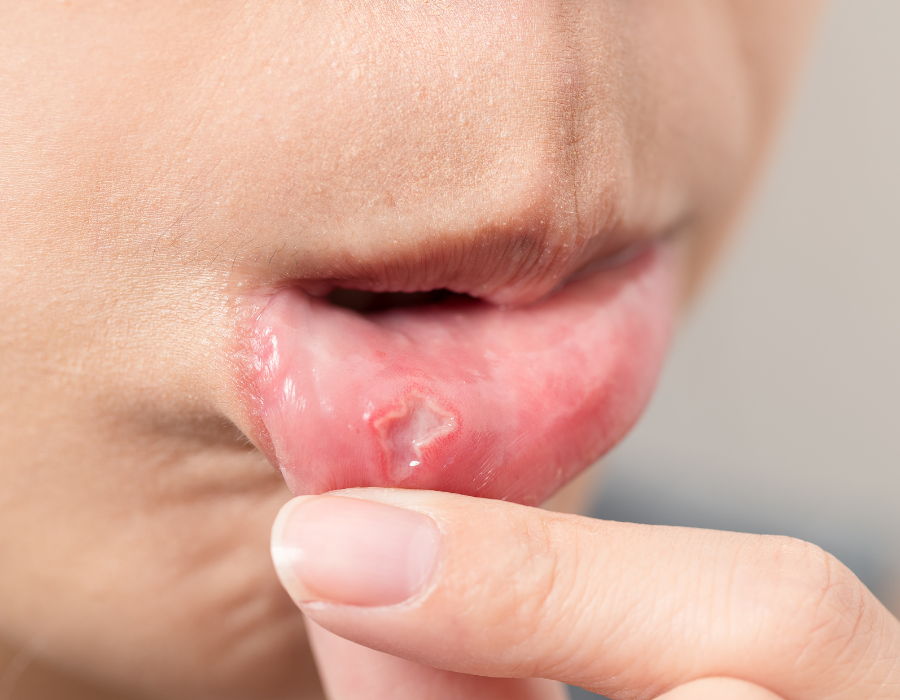
Oral cancer is a serious condition that affected approximately 12,000 people in 2023. It can develop in any part of the mouth or throat, including the lips, tongue, and the floor of the mouth. Unfortunately, oral cancer is often detected in its later stages, leading to a lower survival rate. In fact, the five-year survival rate for oral cancer is only 68%. This makes early detection through regular screenings critically important. At Eggert Family Dentistry, Dr. Elizabeth and Dr. Jeff use the latest technology and techniques to ensure any signs of oral cancer are caught as early as possible, significantly improving the chances of successful treatment.
One of the key messages during Oral Cancer Awareness Month is that anyone can be at risk for this disease. However, certain factors can increase your risk, including tobacco use, excessive alcohol consumption, and exposure to the human papillomavirus (HPV). HPV is now recognized as a significant risk factor for oropharyngeal cancers, which affect the back of the throat, base of the tongue, and tonsils. The rise in HPV-related oral cancers has brought increased attention to the importance of the HPV vaccine as a preventive measure.
What is the HPV Vaccine?
The HPV vaccine is a powerful tool in the fight against oral cancer. It is known as Gardasil 9. It is most effective when administered before individuals become sexually active, which is why it is recommended for preteens, both boys and girls, starting at ages 11 to 12. However, the vaccine can still be beneficial for older teens and young adults up to age 26 who were not previously vaccinated. By ensuring your children receive the HPV vaccine, you can significantly reduce their risk of developing HPV-related cancers later in life.
At Eggert Family Dentistry, Dr. Elizabeth and Dr. Jeff understand that cancer prevention begins with you and your ability to take proactive steps for your family’s health. They encourage you to discuss the HPV vaccine with your child’s healthcare provider and to follow through with the vaccination schedule. Vaccinations are typically available at your local healthcare provider’s office, community health clinics, and sometimes even through school-based programs.
In addition to promoting the HPV vaccine, Dr. Elizabeth and Dr. Jeff emphasize the importance of maintaining regular dental check-ups. These appointments are not just for keeping your teeth clean but also for comprehensive health screenings, including oral cancer detection. By incorporating oral cancer screenings into every recare check-up, they ensure that you receive thorough evaluations that can catch potential issues early, when they are most treatable.
Oral Cancer Awareness Month is a reminder of the significant impact early detection and prevention can have on your health. By visiting Eggert Family Dentistry for your regular check-ups and ensuring your children receive the HPV vaccine, you are taking vital steps toward protecting yourself and your loved ones from the threat of oral cancer. Dr. Elizabeth and Dr. Jeff Eggert are dedicated to providing you with the best care possible and are here to support you in maintaining a healthy, cancer-free life.
Call Eggert Family Dentistry today to make sure you have your family’s next recare visits scheduled. Summer is coming and the schedule fills fast, we want to help keep you on track for all your dental and oral health needs. 651-482-8412.