By: Dr. Elizabeth Eggert
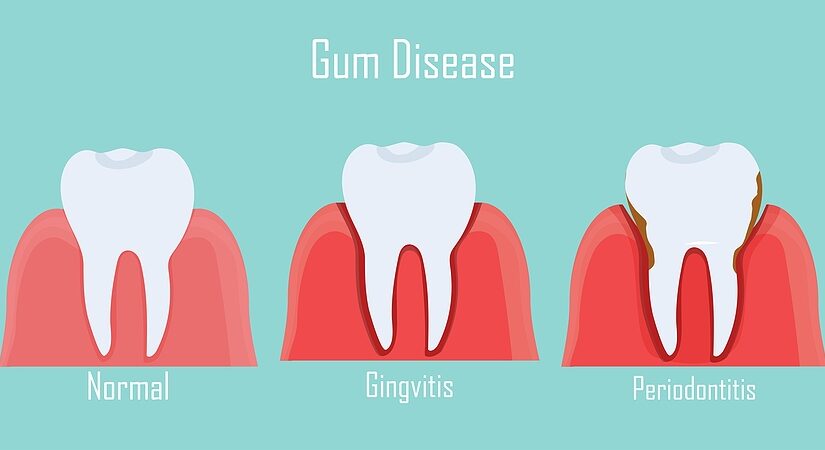
Periodontal diseases are a group of inflammatory conditions affecting the gums and teeth. They range from mild gum inflammation, known as gingivitis, to more severe forms such as periodontitis (gum disease), which can lead to tooth loss if left untreated.
The root cause of periodontal diseases is the proliferation of bacteria on the surface of the teeth, which infects the gums. While deep dental cleanings and oral surgery are key treatments to get rid of bacteria under the gums, non-surgical treatments such as antibacterial therapies are also highly effective.
The Role of Bacteria in Periodontal Diseases
Oral bacteria naturally reside in the mouth, forming a biofilm known as dental plaque. When we don’t keep up consistent oral hygiene practices, this plaque can accumulate and become a breeding ground for harmful bacteria.
These bacteria release toxins and trigger an immune response, leading to inflammation and damage to the gums and supporting structures of the teeth. If left unchecked, the bacterial infection can progress from a mild case of gingivitis to advanced periodontitis, resulting in bone loss and eventual tooth loss.
Non-Surgical Periodontal Treatments:
Non-surgical periodontal treatments aim to remove bacterial plaque and tartar, reduce inflammation, and promote the healing of gum tissues. These treatments are usually the first line of defense against periodontal diseases and may include:
- Scaling and Root Planing: This procedure involves the thorough removal of plaque and tartar from above and below the gumline. It helps to eliminate bacteria and smooth the tooth roots, allowing the gums to reattach to the teeth.
- Antibacterial Mouthwashes: Dentists may prescribe antimicrobial mouth rinses containing ingredients such as chlorhexidine. These rinses can help reduce the bacterial load in the mouth and promote healing.
- Local Antibiotics: In some cases, local antibiotic therapies may be applied directly to periodontal pockets under the gums to eliminate bacteria. This approach enhances the effectiveness of non-surgical treatments like scaling and root planing.
The Role of Antibacterial Therapies in Treating Periodontal Diseases
Antibacterial therapies play a crucial role in combating periodontal diseases by directly targeting the underlying bacterial infection. They can be administered two different ways: systemically and locally.
- Locally Delivered Antibiotics: In most cases, antibiotics are applied directly to the affected areas in the form of topical gels or powders. These topical treatments can be placed into periodontal pockets, localizing the effects of the medication. This approach is usually completed immediately after scaling and root planing procedures.
- Systemic Antibiotics: In severe cases of periodontal diseases, where the bacterial infection has spread extensively, systemic antibiotics may be prescribed for a longer period than average at a low dose. This can enhance the success of deep cleaning procedures. These antibiotics are taken orally and circulate throughout the body to combat bacterial infections.
Think You Need Antibacterial Therapies for Periodontitis?
Non-surgical periodontal treatments, coupled with antibacterial therapies, can help control bacterial infections, reduce inflammation, and promote gum tissue healing. If you think you might require antibiotics to treat periodontitis, come into Eggert Family Dentistry and consult with Dr. Jeff Eggert or Dr. Elizabeth Eggert.
When you schedule an appointment with us, we can assess the severity of the disease and determine whether topical or oral antibacterial therapies are needed. We’ll be able to provide personalized treatment recommendations based on your unique oral health situation. Call us today at 651-482-8412 to schedule an appointment!