By: Dr. Elizabeth Eggert
Periodontal scaling and root planing may sound like a funny way to treat periodontal disease It may even sound a bit intimidating, but this treatment is actually a simple way to immediately start treating gum disease ( periodontal disease). Before we go into an explanation of this procedure, let’s first clarify what gum disease is.
Gingivitis and Periodontitis (Gum Disease)
Gingivitis is an inflammatory reaction of the gums due to excessive bacteria. When you don’t brush and floss regularly, the bacteria surrounding your teeth enters the gums and causes irritation, inflammation, and bleeding of the gums. This can be especially noticeable after brushing or flossing.
Gingivitis can be easily treated with a professional cleaning. If left untreated, however, gingivitis will develop into a serious gum infection called periodontitis, also known as gum disease.
When your gums are chronically inflamed, the space between your gums and your teeth, also known as your gum tissue pockets, gets so deep that the bacteria and plaque become trapped and can no longer be removed with regular brushing or even flossing. Without treatment, gum disease will destroy the bone that supports your teeth. Without the bone to act as a foundation, the teeth get loose and eventually need to be removed.
Symptoms of gum disease include:
- Receding gums
- Gums that bleed after brushing
- Red, swollen gums
- Persistent bad breath
- Loose teeth
- Tooth loss
Aside from damaging one’s oral health, there are other serious risk factors associated with gum disease. It’s long been proven that there is a connection between gum disease and heart disease. In fact, a person with gum disease has two to three times the risk of having a heart attack, stroke, or other cardiovascular event than someone with healthy gums.
For pregnant women, gum disease has also been linked to pregnancy complications and low birth weight.
Treatment for Gum Disease
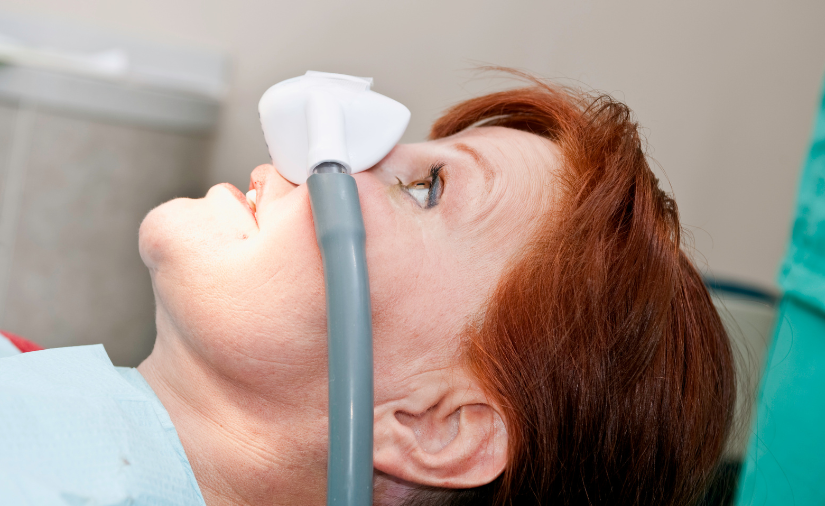
Luckily, the treatment for gum disease is simple and can be performed right here at Eggert Family Dentistry. One of our amazing hygienists along with Dr. Elizabeth or Dr. Jeff will administer treatment known as periodontal scaling and root planing. These procedures are typically quick and can be performed using onlyl local anesthetic.
What is Periodontal Scaling and Root Planing?
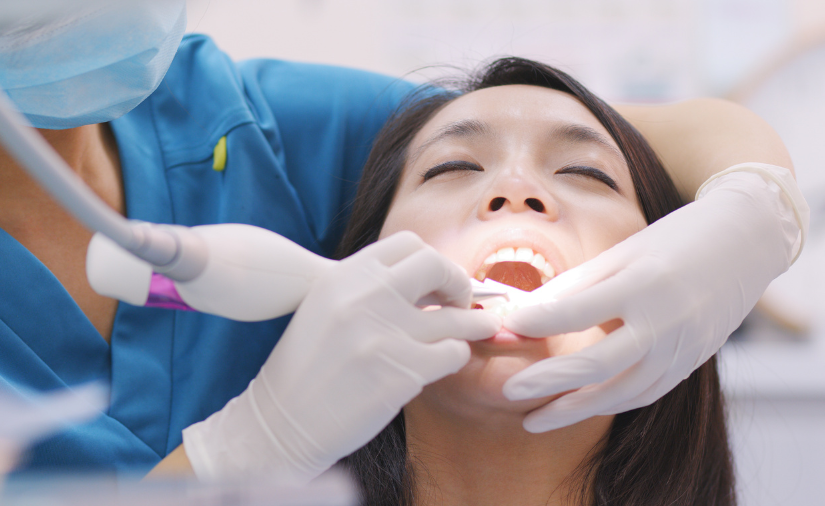
Periodontal scaling is a procedure that uses a dental curette or scaler to remove all the plaque and tartar from above and below the gumline, all the way down to the bottom of the pocket. A topical or local anesthetic will be applied to numb the area so that no discomfort is felt during treatment. Root planing is then when our dental team members use instruments or the high powered water irrigating Cavitron to smooth out the roots of your teeth to help your gums reattach to your teeth. Depending on the severity of the infection, the time needed for these procedures can vary. It is common to complete treatment on one half of the mouth per session.
Aftercare:
After the procedure, you may experience slight tenderness or discomfort with your gums, however, this typically resolves within a couple of days. The full healing process can take weeks, however, as your tissue reattaches to your tooth root.
- To minimize sensitivity, avoid eating sweet items or food that is extremely hot or cold for a few days.
- If you experience any pain while brushing, reduce brushing intensity for at least 48 hours.
- Over-the-counter pain medication will help reduce any discomfort following treatment.
- You can also speed up your recovery by rinsing your mouth with a warm saline solution multiple times a day.
Prevention is Better Than Intervention
Once you have periodontal disease, you will always have periodontal disease, but luckily managing this disease can be straight forward if you follow your recommended recare interval and do your hygiene homework! Typically, a periodontal patient will need a recare visit for a periodontal maintenance cleaning every 3 months.
Don’t Let Gum Disease Get the Best of You
If you’re experiencing any of the symptoms of gingivitis or gum disease, don’t hesitate to contact our office for an appointment. Upon examination, we’ll be able to tell you if it can be remedied with a simple cleaning, or if it requires periodontal scaling and root planing. Call our office to schedule an appointment with us at 651-482-8412.







 While we may tend to villainize sugar, as humans we are biologically predisposed to crave sugary foods and beverages during times in our lives when we need more calories. This is especially true of babies and adolescents whose bodies are growing rapidly. Not only does sugar satisfy a craving and provide the calorie boost growing bodies are looking for, but it has been widely recognized to
While we may tend to villainize sugar, as humans we are biologically predisposed to crave sugary foods and beverages during times in our lives when we need more calories. This is especially true of babies and adolescents whose bodies are growing rapidly. Not only does sugar satisfy a craving and provide the calorie boost growing bodies are looking for, but it has been widely recognized to  When your toddler consumes sugar, it’s often in the form of fruit juice and in some cases, soda. But what actually happens to your child’s teeth when they drink a sugary beverage?
When your toddler consumes sugar, it’s often in the form of fruit juice and in some cases, soda. But what actually happens to your child’s teeth when they drink a sugary beverage?

