By: Dr. Elizabeth Eggert
Smoking is a dangerous habit that can have severe effects on both your overall health and oral health. This is something that research has proven time and time again — and it’s something that the majority of smokers already know.
However, many people are still unaware of the sheer range of problems that smoking can cause. In this blog, we’re taking a look at these health problems, as well as addressing how and why smokers can quit.
While we believe it’s important to inform our patients, we also understand that frightening health facts don’t often help smokers quit. So, if you are considering quitting smoking, but are still on the fence, we encourage you to skip the health section for now, and simply scroll down to our “Why Quit” section, where we discuss the reasons smokers believe they need to smoke. At the end of this article, we also provide you with a list of resources to help you get started on your quitting journey.
Effects of Smoking on Your Overall Health:
When people think of the negative effects of smoking, most people think of the big one: lung cancer. However, because smoking affects nearly every part of the body, it can be the culprit behind a laundry list of illnesses. According to the Center for Disease Control, for every person who dies because of smoking, at least 30 people live with a serious smoking-related illness. Let’s take a deeper look at what smoking does to the body:
Difficulty Breathing:
Smoking causes a range of respiratory problems. When you inhale cigarette smoke, it irritates your airways and causes inflammation, which can make it difficult to breathe. This leads to chronic coughing, wheezing, and shortness of breath. Over time, smoking often leads to chronic obstructive pulmonary disease (COPD), emphysema, and lung cancer.
Increased Anxiety and Depression:
Smoking can also have negative effects on your mental health. Studies have shown that smokers are more likely to experience anxiety and depression than non-smokers. Nicotine acts as a stimulant, increasing feelings of anxiety, while withdrawal symptoms lead to feelings of depression.
Increased Risk of Heart Attack:
Smoking is a major risk factor for heart attack. The chemicals in tobacco smoke damage your heart and blood vessels, leading to an increased risk of heart disease, heart attack, and stroke. In fact, smokers are twice as likely to have a heart attack as non-smokers.
Oxygen Deprivation of All Muscles:
When you smoke, the nicotine in tobacco causes your blood vessels to narrow, which restricts blood flow and oxygen to your body. This leads to oxygen deprivation in every single muscle of the body, which causes chronic fatigue, poor wound healing, and peripheral artery disease.
Effects of Smoking on Your Oral Health:
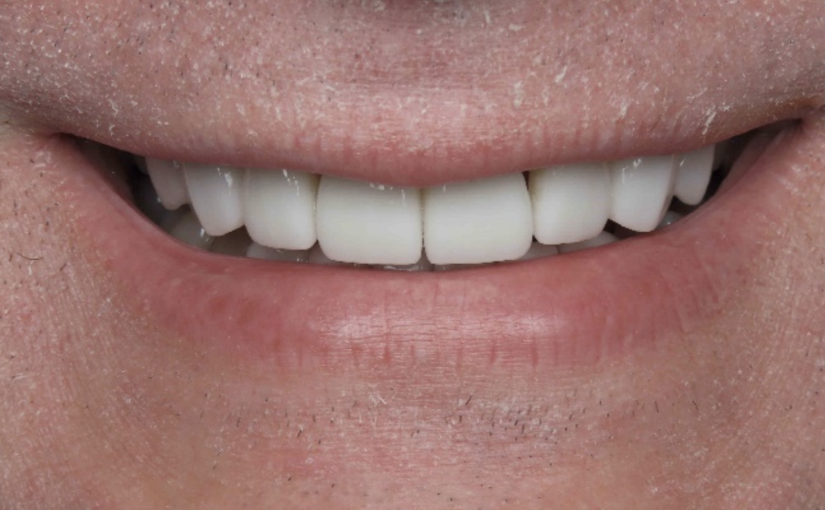
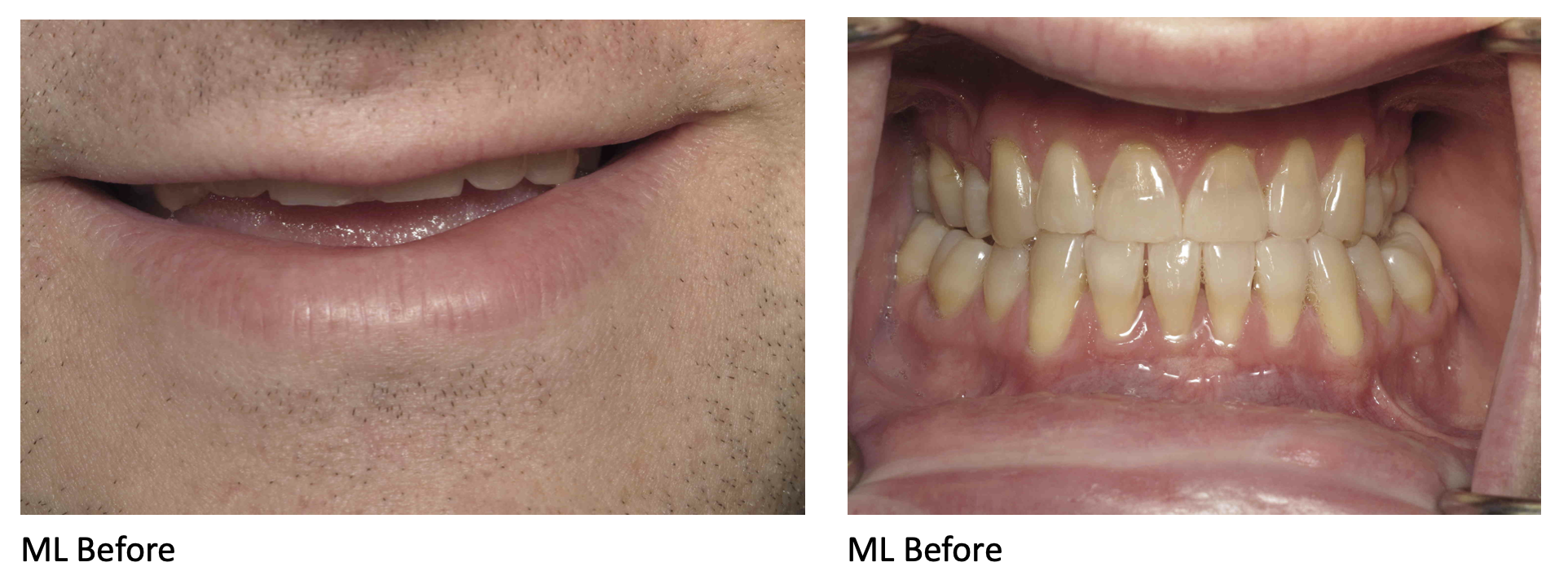
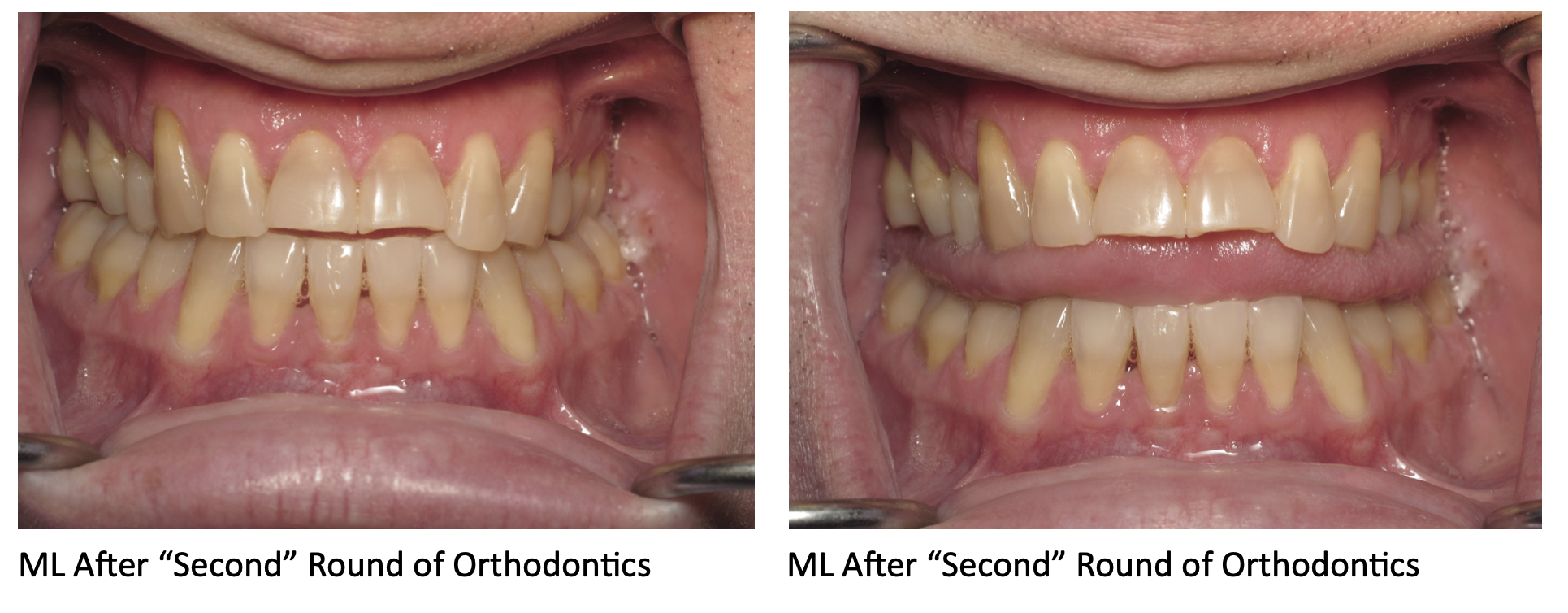
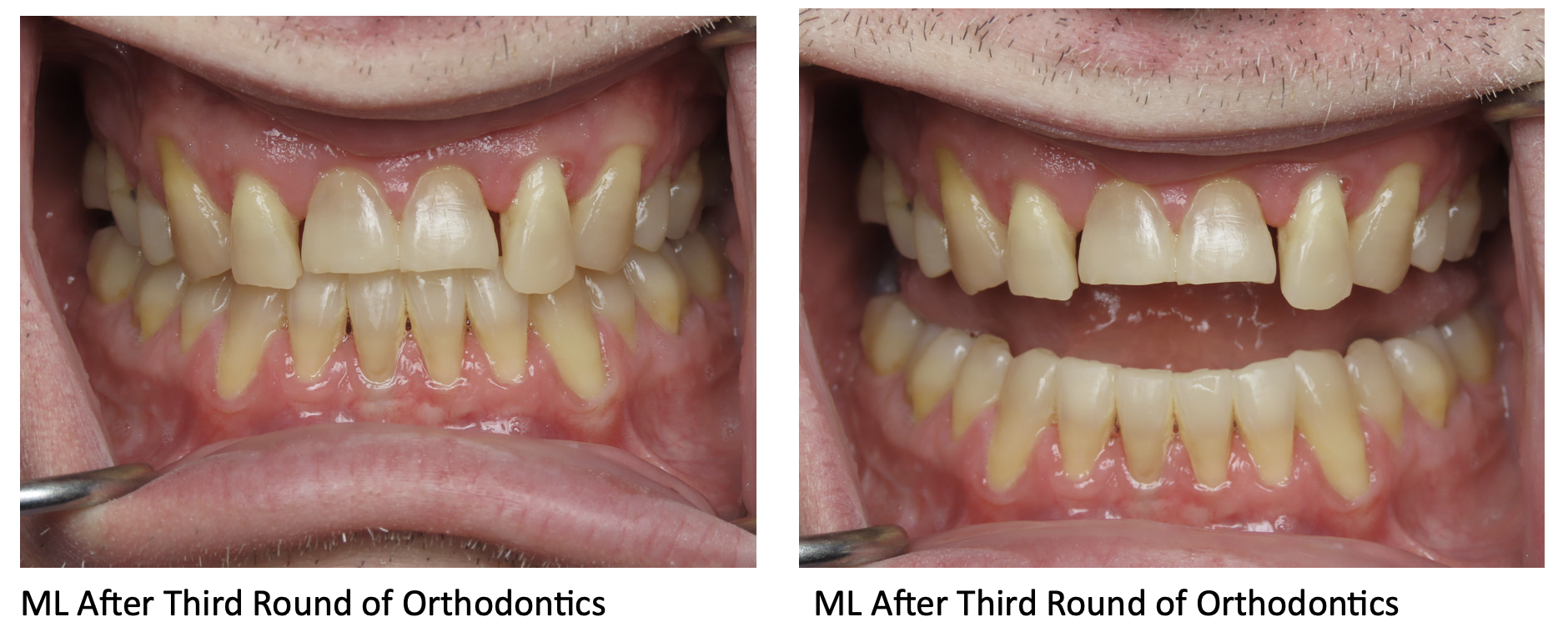
Yellowed Teeth:
One of the most visible effects of smoking on your oral health is yellowed teeth. The tar and nicotine in tobacco smoke will stain your teeth, giving them a yellow or brownish hue. This staining is usually unsightly and difficult to remove.
Dry Mouth:
Smoking also causes dry mouth, which occurs when there is a decrease in the production of saliva. Saliva plays an important role in keeping your mouth healthy by washing away food particles and neutralizing acids produced by bacteria. When you have a dry mouth, you are more susceptible to tooth decay and gum disease.
Receding Gums:
Smoking can also lead to receding gums, which is when the gum tissue around your teeth pulls back, exposing the roots of your teeth. This can cause tooth sensitivity, as well as an increased risk of tooth decay and tooth loss.
Increased Cavities and Tooth Loss:
Smoking also increases your risk of cavities and tooth loss. The chemicals in tobacco smoke can damage the enamel on your teeth, making them more susceptible to decay. Additionally, smoking can lead to gum disease, which is a major cause of tooth loss.
Oral Cancer:
Some of the chemicals contained in tobacco smoke and chewing tobacco are carcinogenic, meaning they cause genetic changes in cells of the mouth cavity and cause oral cancer. Regular dentist visits are a must if you’re worried about developing oral cancer, as Dr. Jeff Eggert or Dr. Elizabeth Eggert can provide thorough oral cancer screenings as a part of our proactive approach to dentistry.
In conclusion, smoking has a range of negative effects on your overall health and oral health. Quitting smoking is the best way to reduce your risk of developing these health problems and improve your overall well-being.
Why Quit?
Every smoker knows they should quit for the detrimental health risks. And yet every smoker wants to continue smoking. So, before we talk about quitting, it’s important that we first address why smokers smoke in the first place — or why they believe they have to smoke.
Smokers usually cite a number of reasons for why they smoke, including:
- Stress: Smokers believe that smoking relieves stress or calms them down.
- Boredom: Smokers believe that they smoke because they are bored.
- Concentration: Smokers believe that smoking helps them concentrate.
Because they hold these beliefs about what smoking does for them, smokers are under the impression that quitting smoking would rob them of these supposed “benefits” of smoking. The wonderful truth is, smoking does none of these things for you.
Smoking doesn’t calm you down. In fact, it does quite the opposite. Nicotine is a known stimulant that raises your heart rate and blood pressure, causing increased stress and anxiety in both the short and long-term.
Smoking doesn’t relieve boredom. When smokers are bored, it’s true that they often light a cigarette. However, smoking cigarettes itself isn’t exciting. If you weren’t a smoker, chances are you’d find something else to do that would be significantly more entertaining than inhaling cigarette smoke for seven minutes.
Smoking doesn’t help you concentrate. Research confirms that smoking is terrible for your concentration. Having a nicotine addiction – or any addiction, for that matter – is incredibly distracting, and makes it much more difficult to concentrate on day-to-day tasks.
So, to the question “Why quit?” We answer:
- To be free of nicotine addiction.
- To experience a vastly improved bill of health.
- And because smoking does nothing for you in the first place. You have nothing to lose!
Resources to Help You Get Started with Quitting Smoking
Allan Carr’s “EasyWay To Stop Smoking”: Developed by a former chainsmoker, this smoking cessation technique uses a combination of logic and psychology to break down all the reasons why smokers believe they need to smoke, and then explodes each myth one by one. (For example, our points in the above section were taken from Allan Carr’s work.) Carr’s method is available in print, as an audiobook, or in-person as a seminar.
National Cancer Institute Quitline: The National Cancer Institute provides a free smoking cessation hotline where people can receive counseling and support to quit smoking. The Quitline can be reached at 1-877-44U-QUIT (1-877-448-7848).
Smokefree.gov: Smokefree.gov is a website created by the U.S. Department of Health and Human Services that provides a range of resources to help people quit smoking, including a step-by-step quit guide, mobile apps, and text message support.
American Lung Association: The American Lung Association offers a range of resources to help people quit smoking, including online tools, support groups, and a free quit smoking helpline at 1-800-LUNGUSA (1-800-586-4872).
Your healthcare provider: Your healthcare provider can provide guidance on quitting smoking and may be able to prescribe medications or recommend other treatments to help you quit smoking.
Community resources: Many communities have resources to help people quit smoking, including local support groups, smoking cessation programs, and community health clinics. Check with your local health department or community center to find out what resources are available in your area.
Lean on The Experts at Eggert Family Dentistry
The negative health effects of smoking are vast and far-reaching, impacting both overall health and oral health. However, quitting smoking is the single most important step you can take to improve your health and wellbeing. If you or someone you know is struggling with smoking cessation, there are many resources available to help you on your journey.
At Eggert Family Dentistry, we are committed to helping our patients achieve optimal oral health. If you have questions or need assistance with smoking cessation, please don’t hesitate to reach out to us at 651-482-8412. Our team is here to support you on your journey to a healthier, smoke-free life!