By: Dr. Elizabeth Eggert
How did this start?
Ann returned to Eggert Family Dentistry a few years ago after concerns arose at her previous dental office, where she often felt she was being “up-sold” on dental recommendations. In addition, her husband and mom have been patients at Eggert Family Dentistry for years and have been very happy with their experiences. Ann made it very clear from the start that her main concern is overall tooth health, and while she wants a beautiful smile, she is happy with her smile, so she didn’t feel the need to discuss cosmetic options. Ann mentioned at her new patient appointment that she had undergone a sleep study and she was told she didn’t have sleep apnea, but she has been told she snores so she wonders if she is as rested as she could be. She was also told by her previous dentist that she had “TMJ” or Temporal Mandibular Joint Disorder (TMD) and wanted Dr. Elizabeth’s opinion on that. Ann really didn’t have many symptoms of TMD and she wanted to better understand what the previous dentist was seeing.

What was revealed during the records process?
Dr. Elizabeth invited Ann to come back for The Records Process in order to help Ann understand her current dental conditions, including the status of her potential TMD. In the Records Process, we used models, photos, and x-rays, as well as results from an extensive analysis of how Ann’s teeth function. The details of The Records Process revealed that Ann had some evidence of an unstable bite and while it wasn’t causing Ann day-to-day problems, it has the potential to cause faster breakdown of her jaw joints, muscles, and teeth. In addition, with her snoring, Ann had the option of working through the Seattle Protocol, an innovative approach to treating sleep disordered breathing with dental resources, like dental splints. Even though Ann did have evidence of TMD (without current symptoms), she wasn’t interested in pursuing treatment for that, which may have included orthodontics, but she was interested in helping her snoring, so she elected to undergo the Seattle Protocol.

What was involved?
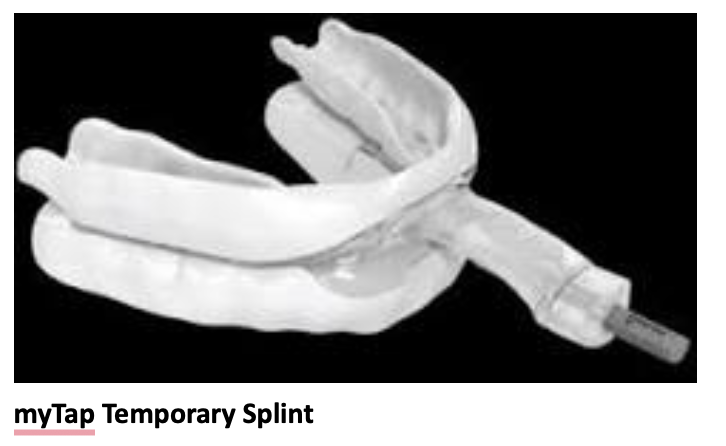
The Seattle Protocol helps us determine the jaw position that best alleviates the patient’s likely airway compromise. The protocol moves the patient through a series of diagnostic steps and treatments using various trial splints (using the myTap system) to find the most effective solution specific to each individual patient. The goal is to move through incremental vertical and horizontal increases to the jaw position. Each step builds upon the last, but patients don’t necessarily need to complete the entire process as the purpose of the protocol is to determine the phase that provides the best relief of the patient’s symptoms.
Seattle Protocol Six Steps
1. Nasal breathing therapy
2. Lower jaw orthotic trial splint
3. Lower jaw anterior repositioning trial splint
4. Dual arch trial splint
5. Dual arch repositioning trial splint
6. Dual arch repositioning trial splint in more forward position.
For Ann, like all patients starting with the Seattle Protocol, we started with Nose Clearing and Mouth Taping, with the goal of rerouting Ann’s breathing through her nose. Ann ended up moving through the first 4 stages and found relief from her snoring and reported sleeping better with stage 3.

What does Ann think?
We asked Ann what she thought about the process of undergoing the Seattle Protocol. She told us she found it very easy and the time went pretty quickly. “Both Dr. Eggert and Tracy helped me move fast through the treatment and my appointments always went smoothly and started on time.” She also found it to be really helpful and that the mouth taping was very beneficial, she even recommended it to some of her friends that she felt it would help.
Ann liked the different options of oral appliances and finding the right one for her after going through all the Seattle Protocol. We asked Ann what she would tell a friend or family member if they were having similar symptoms or issues and she said that she would highly recommend the treatment and working with Eggert Family Dentistry. “You really have to sleep on it! Literally, you have to sleep with the different splints as it is not possible to know how they will benefit you until you try them out. If one version does not work for you, you will know it.”
Congratulations Ann! Thank you for letting us be part of your journey. We’re happy to have found a conservative treatment option that addresses your goals and current conditions. We look forward to working with you and your family for many more years to come!










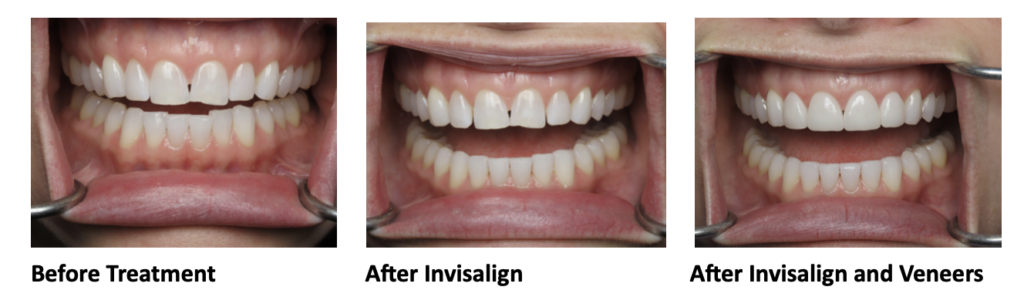
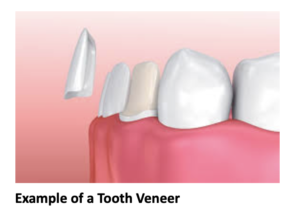
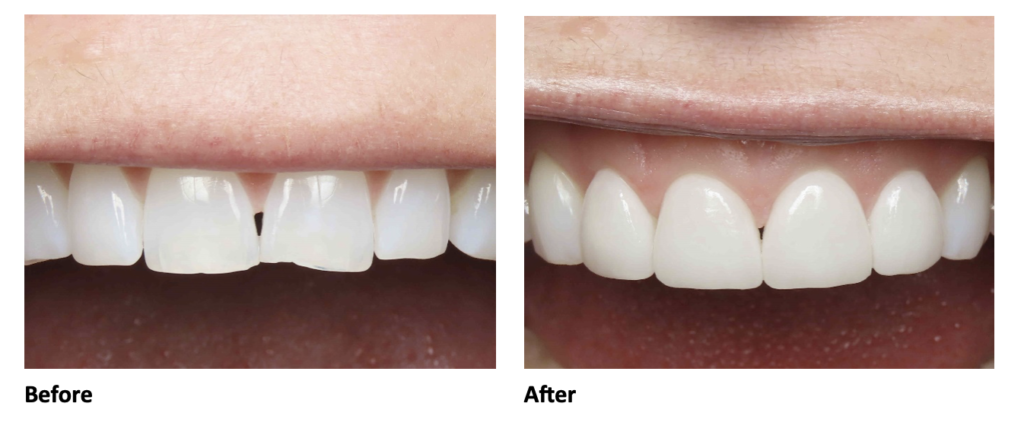
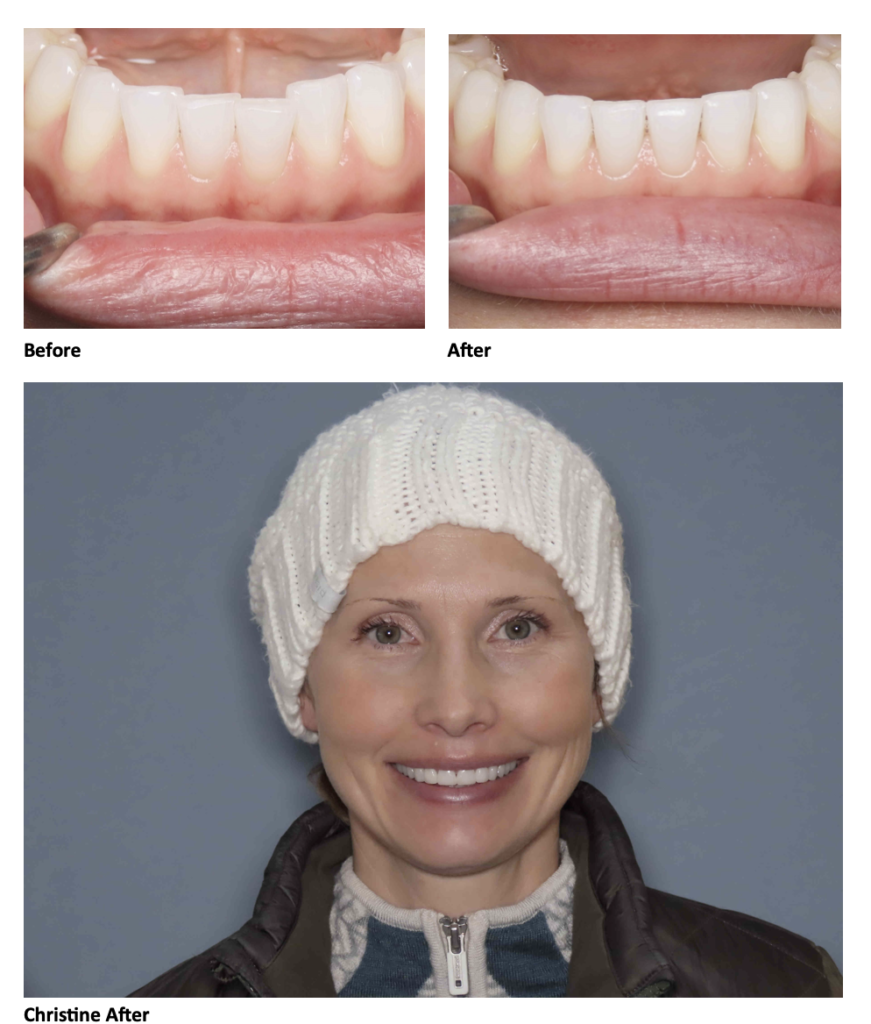

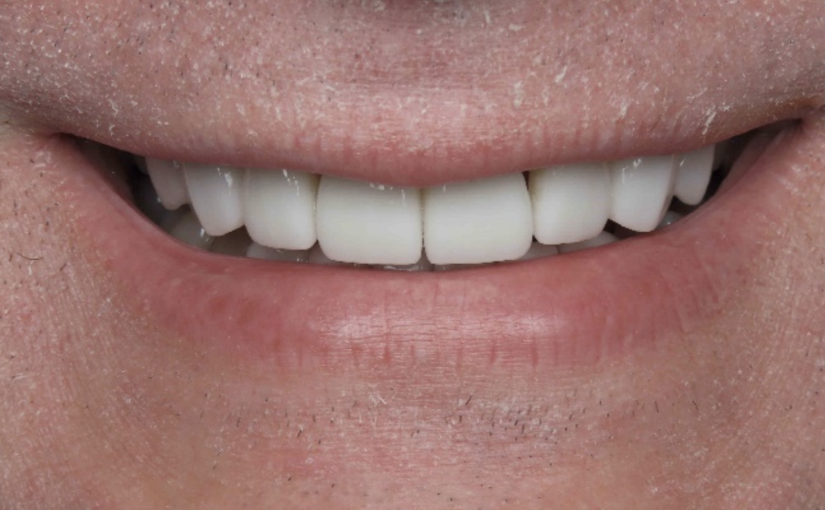
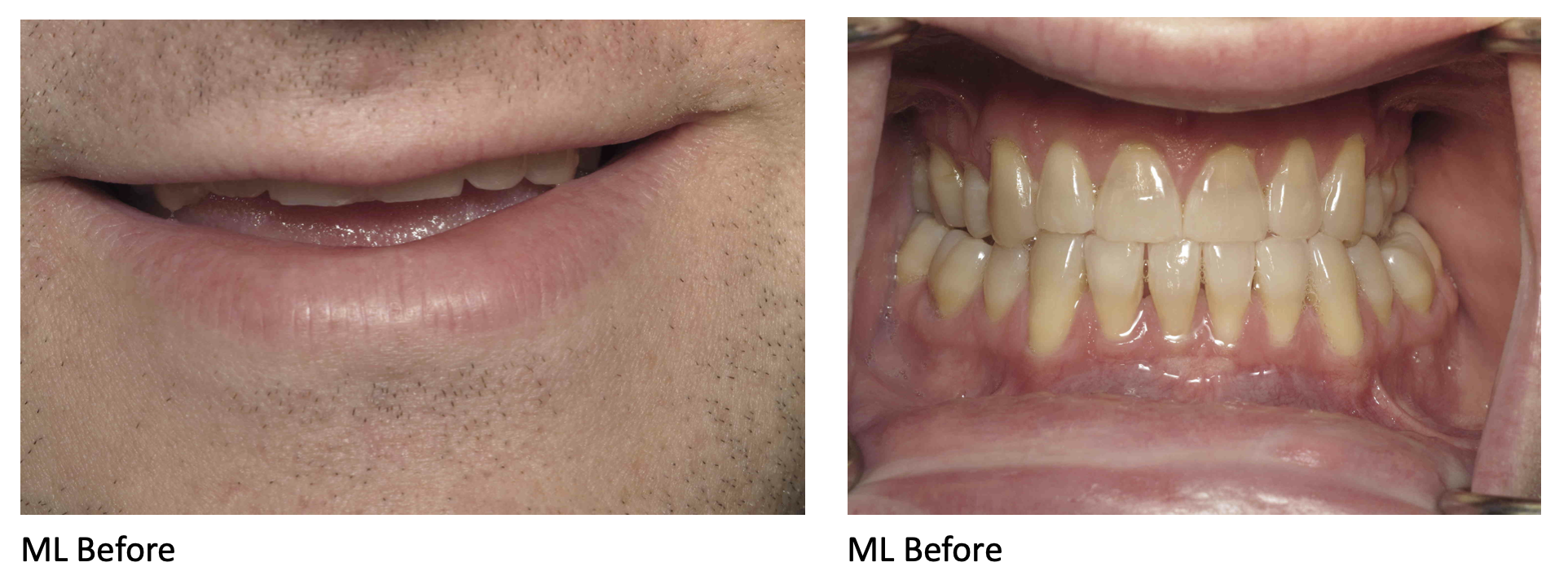
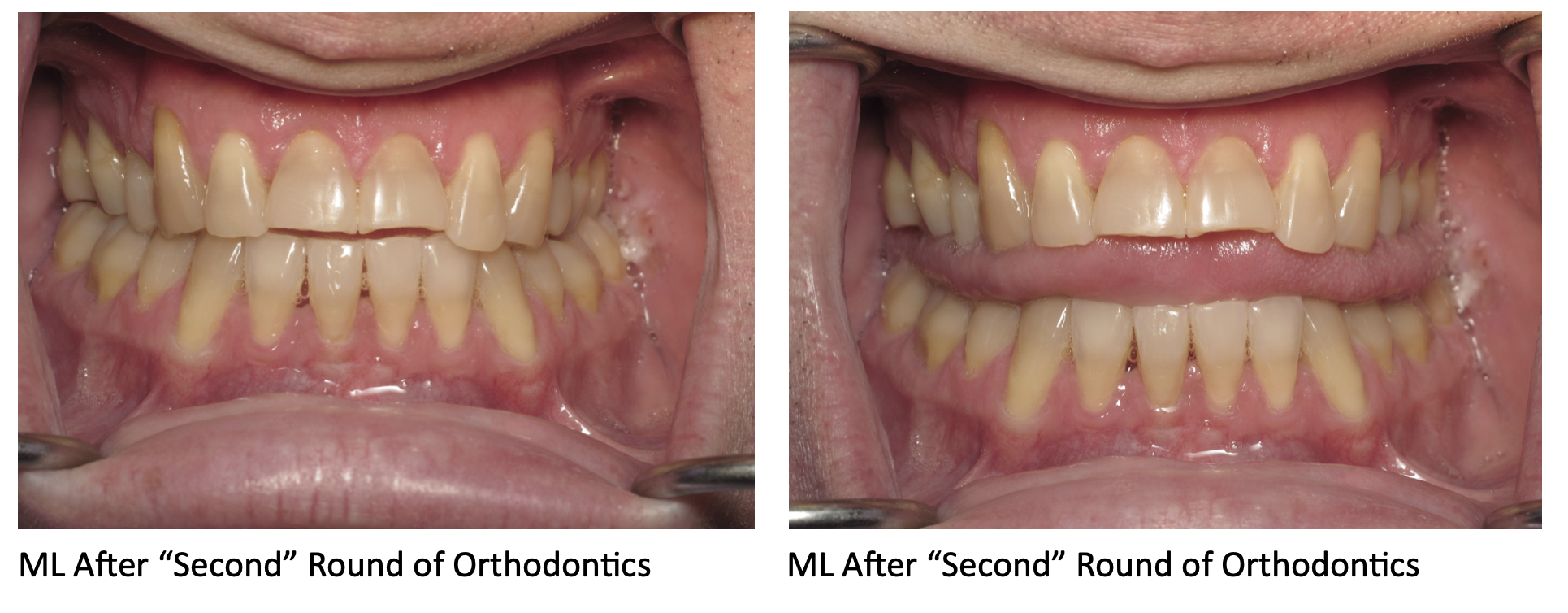
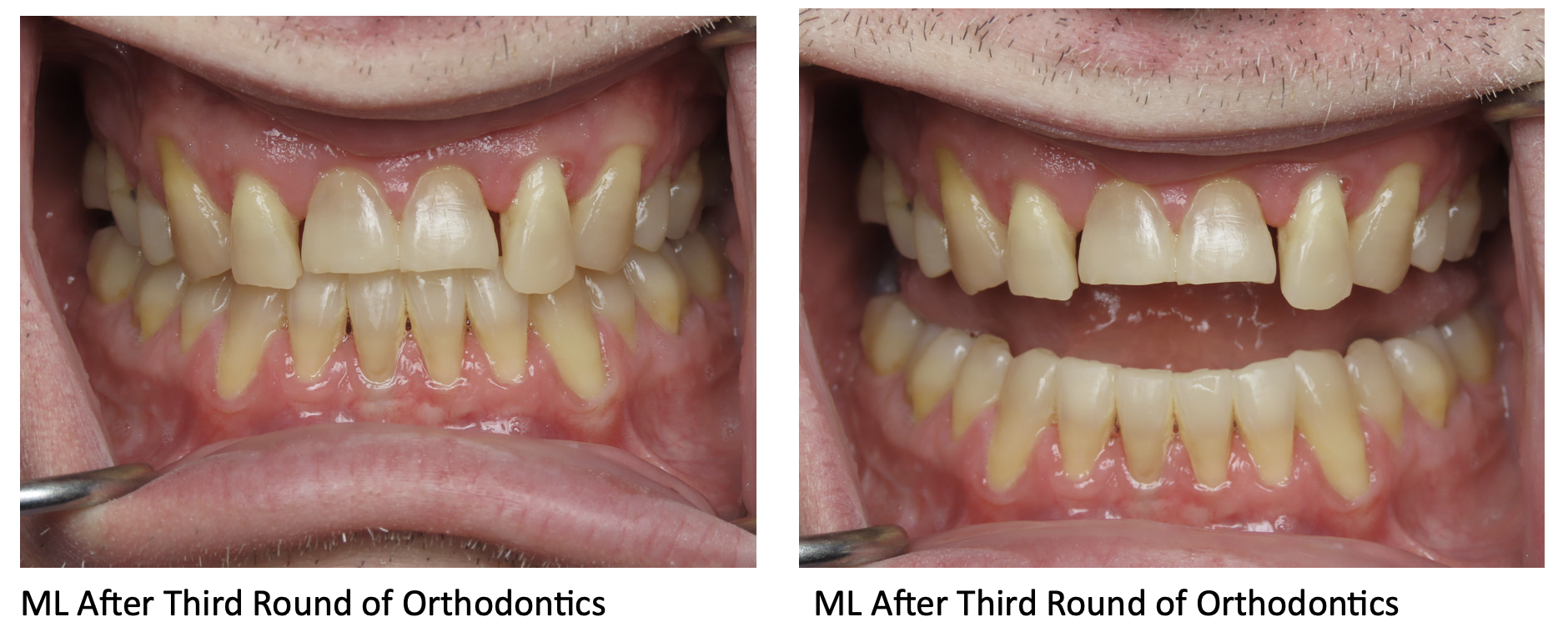
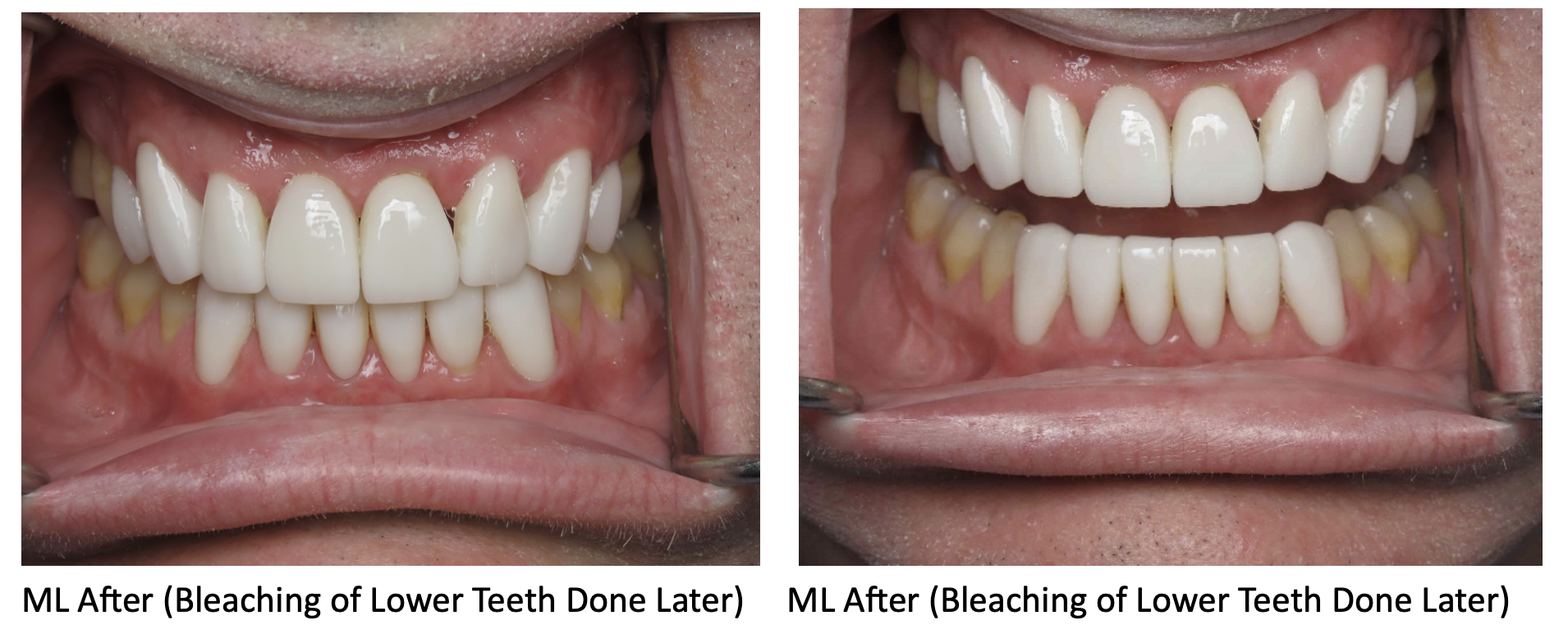
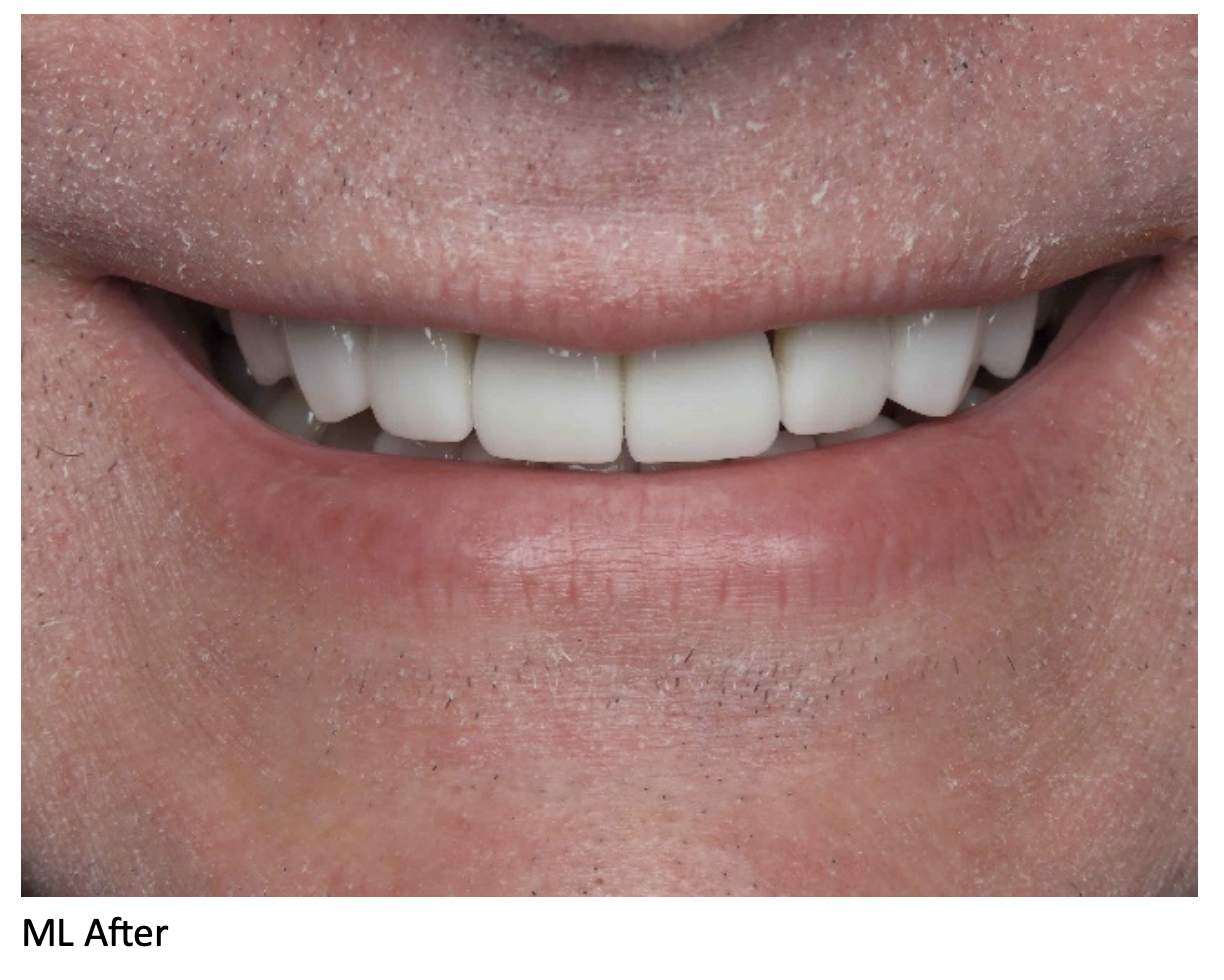





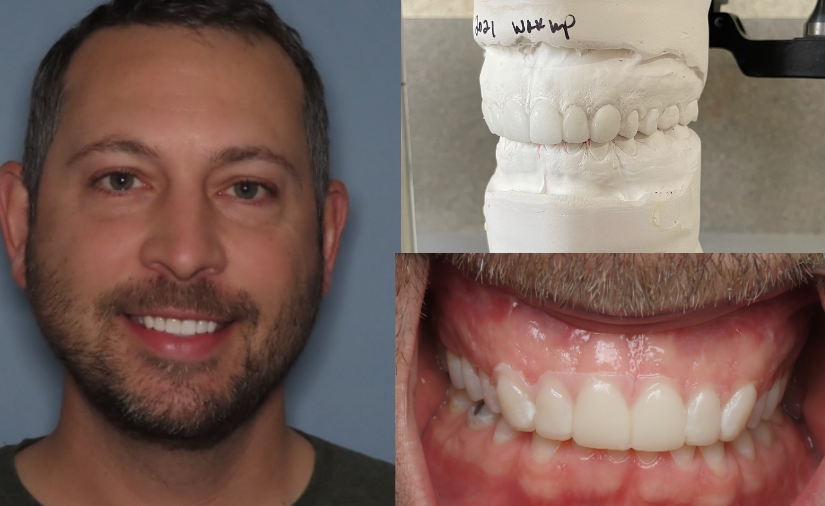
 For example, our patient “M” had recently undergone corrective jaw surgery, but was still experiencing issues with his bite. To make sure we got a holistic picture of M’s oral issues post-op, we put him through the records process and were able to determine that he needed to have his front teeth lengthened slightly to correct his occlusal imbalance. (
For example, our patient “M” had recently undergone corrective jaw surgery, but was still experiencing issues with his bite. To make sure we got a holistic picture of M’s oral issues post-op, we put him through the records process and were able to determine that he needed to have his front teeth lengthened slightly to correct his occlusal imbalance. (
 If the records process is the “blueprint” for your treatment plan, then the
If the records process is the “blueprint” for your treatment plan, then the