By: Dr. Elizabeth Eggert
In the immediate hours after getting a dental crown, you may wonder, “What did Dr. Eggert say again? Are there supposed to be any restrictions for me today?” Well, wonder no more. Here we will share several post-operative care measures that can contribute to a smoother recovery and enhance the longevity of your crown as well as improve your healing.
You maybe didn’t know, but our website has helpful post-operative instructions for most of the dental procedures done in our office including Crowns.
After the Preparation Appointment
After the preparation appointment, if you did not have a CEREC crown done, you are wearing a temporary crown or bridge. This is held on with temporary cement. Be sure to avoid sticky foods and gum so as to not pull the temporary off. Also avoid hard or crunchy foods. It is best to chew on the opposite side as much as possible.
Expect your gum tissues to be sore for a few days. It helps to rinse with warm salt water (8 oz warm water and 1 teaspoon salt) 2-3 times daily for 3-5 days. It also helps to take some over-the-counter pain medication like ibuprofen or Tylenol for both gum soreness, tooth soreness, and jaw soreness. Take that as directed in our office, for most patients that are able to take ibuprofen, we will recommend 600 mg of ibuprofen every 6 hours for the first 1-5 days.
It is important to brush and floss the temporary. This will help the gum tissues heal faster. Brush with small, circular, massaging strokes along the gumline. While flossing, pull the floss out to the side if you experience a lot of resistance through the contact point of the tooth. Occasionally temporary crowns will be splinted together, or in the case of a temporary bridge, use the floss threader as directed in our office.
Temporary crowns rarely come loose, but if yours happens to do so:
- Don’t panic and try to save the temporary (i.e. don’t swallow it)
- Attempt to re-fit the temporary on your tooth using toothpaste to hold it in place
- Call our office right away to find a time for us to recement your temporary for you
What Are Some Symptoms I Should be Concerned About?

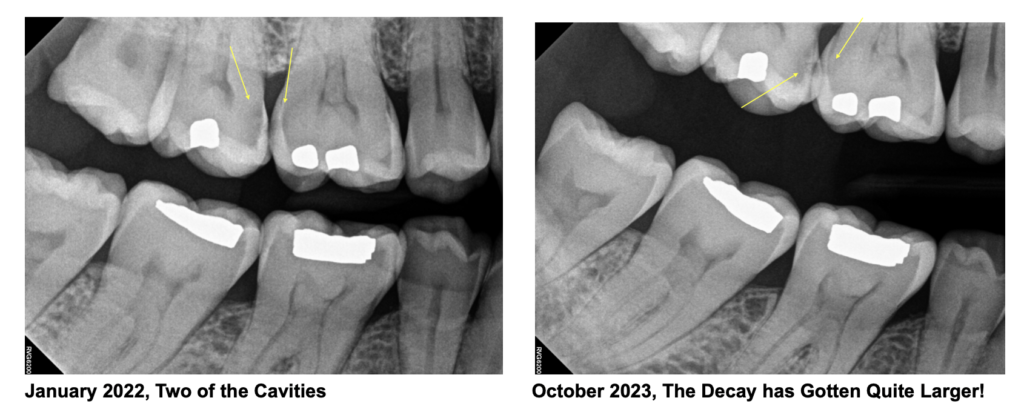
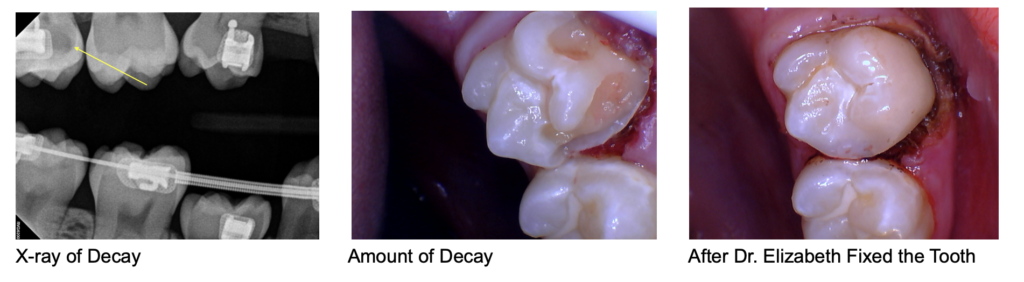
Occasionally teeth undergoing the preparation procedure will experience inflammation in the nerve. This can happen with any tooth, but more commonly occurs in a tooth that has had a large filling or deep decay, cracking, fracture, or pain before the preparation procedure. The inflammation in the nerve tissue can become irreversible, necessitating additional procedures for the tooth. If you have any of the following signs or symptoms, call our office right away:
- Prolonged pain after cold, hot, or chewing that gets worse over time
- A dull ache that won’t go away
- The need to take over-the-counter pain medicine for 5 days or more “around the clock”
- Pain that wakes you up at night
- Pain that gets worse over time instead of better
- Swelling getting worse in the gums or tissues surrounding the tooth
After the Cementation Appointment
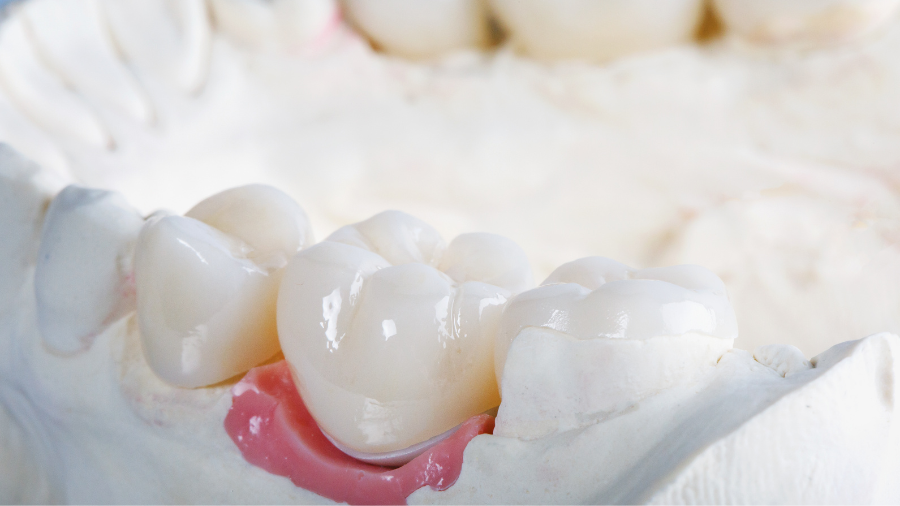
After the cementation appointment, the gum tissues and tooth may be sensitive and sore for a couple of days. Use warm salt water rinses and over-the-counter pain medicine during this time if needed. Brush and floss the new crown or bridge as you would any tooth. If you experience any of the signs or symptoms listed above describing inflammation in the nerve, please call our office right away. If you had a CEREC crown done, your preparation and cementation occurred all in one day. The same instructions apply although there is no need to avoid sticky or crunchy foods.
Generally, you may want to avoid eating or drinking for a couple of hours after the procedure so you don’t accidentally bite your cheeks, lips, or tongue due to the local anesthetic used for your procedure. It is also helpful to stick with easy to chew foods to minimize the stress for your tooth.
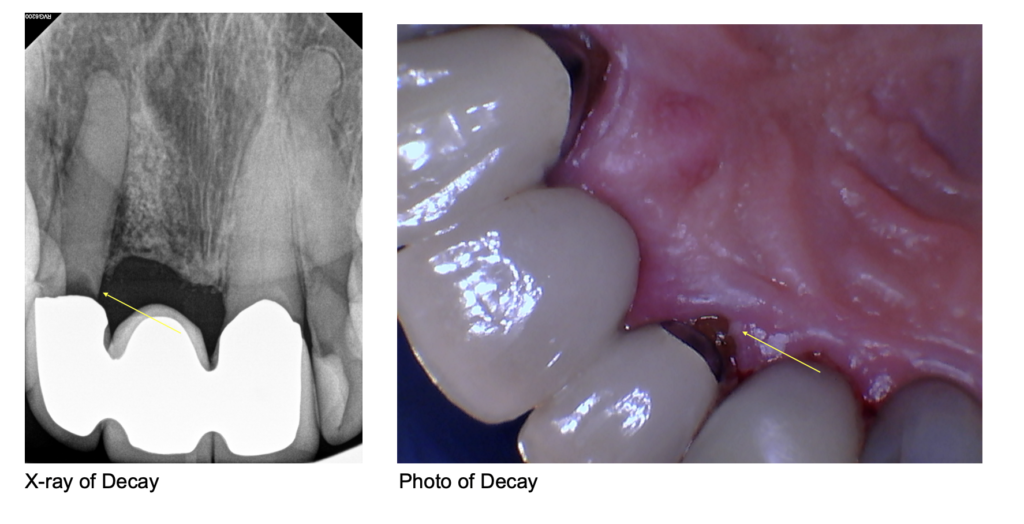
Once you have your final crown, practicing good oral hygiene remains essential. It still is possible to get decay and gum disease even if your tooth has a crown.
After the placement of a dental crown, certain restrictions and considerations should be observed to ensure the optimal success and longevity of the restoration. While dental crowns are designed to restore the function and esthetics of a damaged tooth, it’s important to be mindful of so your crown can last for many years!
Eggert Family Dentistry, Your Dental Crown Experts
We’re here for you if you still have questions about what to do after your dental crown procedure. Call our office today at 651-482-8412! We look forward to working with you again soon!

![Do I Need a Dental Crown? [Answered]](https://blog.eggertfamilydentistry.com/wp-content/uploads/2023/11/Do-I-need-a-crown-answered-825x506.png)