By: Dr. Elizabeth Eggert
How Did This Start?
Tom’s journey began in 2014 when he came to us as a new patient looking to improve his oral health and the appearance of his teeth. During his comprehensive exam, Dr. Elizabeth found the main areas of concern to be the excessive wear, erosion and fracturing of Tom’s teeth. Dr. Elizabeth recommended Tom go through the records process (you can learn more about the records process here) and based on the information gathered during that process, she recommended a full-mouth reconstruction to address his uneven bite and rebuild his broken teeth. Throughout the process of reconstruction, it became clear that the amount of force in Tom’s bite was putting too much pressure on even his temporary crowns, which resulted in the temporaries cracking or falling out on more than one occasion. Dr. Elizabeth was concerned that even after completing the full mouth reconstruction, Tom would have underlying issues. Given Tom’s other symptoms, including difficulty breathing through his nose, dry mouth and use of a CPAP machine, Dr. Elizabeth recommended Tom complete the Seattle Protocol to help address his airway patency.
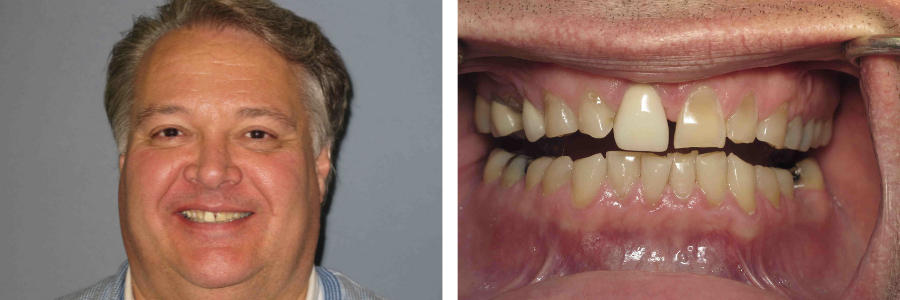
What Was Involved?
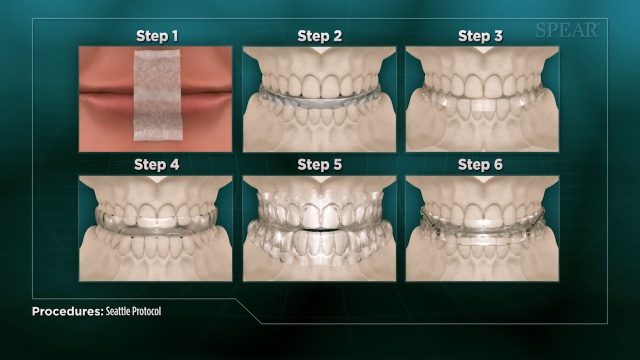
The Seattle Protocol is a six-step process that helps patients with symptoms of sleep-disordered breathing and other conditions determine whether a compromised airway is contributing to their ailments. Each step builds upon the last, but patients don’t necessarily need to complete the entire process as the purpose of the protocol is to determine the phase that provides the best relief of symptoms. You can learn more about the Seattle Protocol and each of the steps here. Throughout the process, Tom noticed improvements in his symptoms such as dry mouth, decreased clenching and grinding, and less waking throughout the night.
What Have Tom’s Results Been?
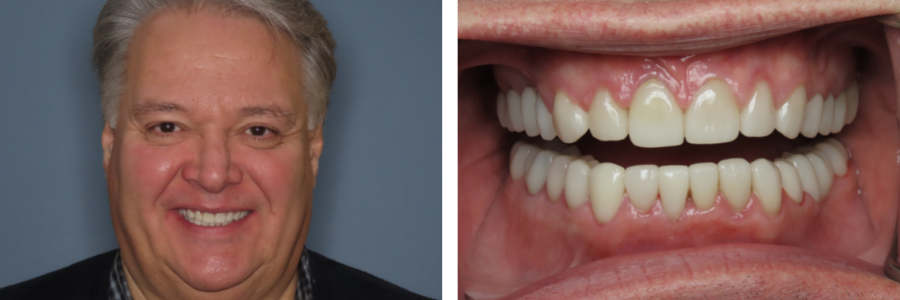
After completing five of the six steps of the Seattle Protocol, Dr. Elizabeth fabricated a sleep appliance for Tom to continue to improve his airway patency, reduce his bruxism and help him sleep better. Tom has now been using his sleep appliance for over a month and says the results so far have been great! He’s noticed less clenching and jaw pain and experienced an overall improvement in his sleep. Tom said that going through the Seattle Protocol helped him better understand the connection between his sleep and airway issues and he appreciates Dr. Elizabeth’s thorough explanation and care throughout each stage.




 The first time we see you for sleep apnea symptoms, we will perform an assessment for signs of structural abnormalities or any physical issues that could be contributing to airway obstruction. This could include an enlarged tongue or tonsils, a small jaw or a large neck.
The first time we see you for sleep apnea symptoms, we will perform an assessment for signs of structural abnormalities or any physical issues that could be contributing to airway obstruction. This could include an enlarged tongue or tonsils, a small jaw or a large neck.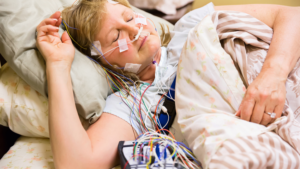 A
A 
 When you come in for an appointment, we look for signs or symptoms that could be considered “red flags” for airway conditions, including sleep apnea. Dr. Elizabeth or Dr. Jeff perform an assessment to see if you have any of the following risk factors among many others:
When you come in for an appointment, we look for signs or symptoms that could be considered “red flags” for airway conditions, including sleep apnea. Dr. Elizabeth or Dr. Jeff perform an assessment to see if you have any of the following risk factors among many others: Did you know that, in
Did you know that, in  Bruxism is another condition that is often present alongside obstructive sleep apnea. Often intertwined with TMD, bruxism describes a condition caused by the clenching or grinding of teeth. It occurs unconsciously during sleep and can be another way a person’s body compensates for an airway obstruction.
Bruxism is another condition that is often present alongside obstructive sleep apnea. Often intertwined with TMD, bruxism describes a condition caused by the clenching or grinding of teeth. It occurs unconsciously during sleep and can be another way a person’s body compensates for an airway obstruction.


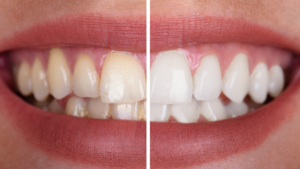 Teeth whitening: Over time, teeth become stained from certain foods, beverages, medications and smoking. Eggert Family Dentistry has many great options to help restore your pearly whites. We provide professional-grade strips and whitening trays that are more effective and gentler on your teeth and gums than their over-the-counter counterparts. Dr. Elizabeth and Dr. Jeff also offer the Zoom and
Teeth whitening: Over time, teeth become stained from certain foods, beverages, medications and smoking. Eggert Family Dentistry has many great options to help restore your pearly whites. We provide professional-grade strips and whitening trays that are more effective and gentler on your teeth and gums than their over-the-counter counterparts. Dr. Elizabeth and Dr. Jeff also offer the Zoom and 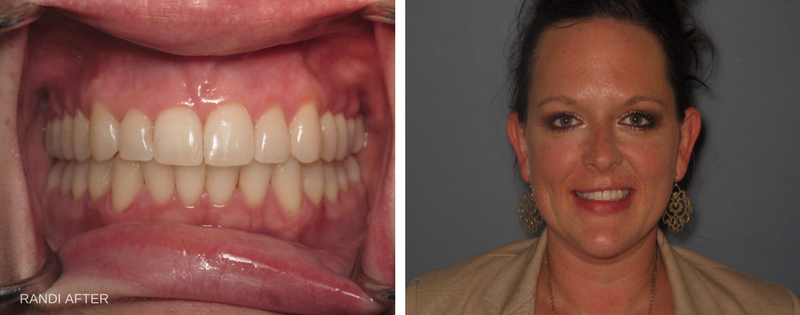
 Tooth replacement: Losing permanent teeth can happen from trauma to the jaw, from gum disease or from tooth decay. Regardless, it can be an awkward situation and one that most people want to remedy as quickly as possible. If you’re dealing with missing permanent teeth, you have some excellent options. These options include dental implants, bridges, partial dentures or full dentures.
Tooth replacement: Losing permanent teeth can happen from trauma to the jaw, from gum disease or from tooth decay. Regardless, it can be an awkward situation and one that most people want to remedy as quickly as possible. If you’re dealing with missing permanent teeth, you have some excellent options. These options include dental implants, bridges, partial dentures or full dentures. Full Dentures: Full dentures are full sets of upper and/or lower artificial teeth that are suctioned into place and removable for cleaning. While they can take some getting used to, they start to feel more normal over time. Full dentures will eventually become loose as bone mass degrades.
Full Dentures: Full dentures are full sets of upper and/or lower artificial teeth that are suctioned into place and removable for cleaning. While they can take some getting used to, they start to feel more normal over time. Full dentures will eventually become loose as bone mass degrades.
 It’s not disputed that whiter teeth lend themselves to a more attractive smile. Statistically,
It’s not disputed that whiter teeth lend themselves to a more attractive smile. Statistically,  Avoid foods and beverages that stain teeth:
Avoid foods and beverages that stain teeth: 
 Practice daily dental care: The single best way to prevent tooth discoloration is by brushing and flossing faithfully each day. Brush in the morning and evening (more often if you eat sugary, acidic, or highly pigmented foods) and floss at least once a day. Additionally, you can incorporate a daily swish of fluoride mouthwash to cleanse your mouth from residual food particles and bacteria and keep enamel strong.
Practice daily dental care: The single best way to prevent tooth discoloration is by brushing and flossing faithfully each day. Brush in the morning and evening (more often if you eat sugary, acidic, or highly pigmented foods) and floss at least once a day. Additionally, you can incorporate a daily swish of fluoride mouthwash to cleanse your mouth from residual food particles and bacteria and keep enamel strong. Zoom Whitening: Another popular option we offer at Eggert Family Dentistry is
Zoom Whitening: Another popular option we offer at Eggert Family Dentistry is 