By: Dr. Elizabeth Eggert
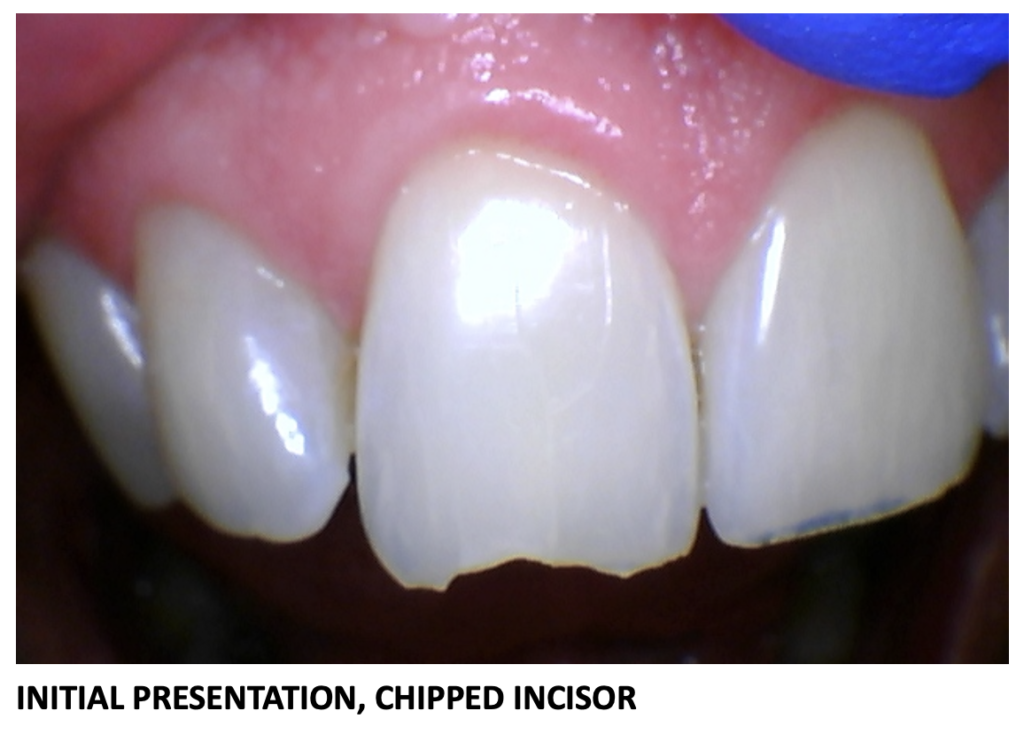
Teeth take a lot of wear and tear and over time, can become fractured, cracked, and decayed. Early intervention is the best way to save your tooth and prevent more serious issues. Dr. Elizabeth Eggert and Dr. Jeff Eggert often recommend dental crowns for patients with these tooth issues. As we all know, any good investment is worth protecting, and crowns are no exception. It’s important to be proactive to ensure crown longevity.
What is a dental crown, and how does it work?
Before we get into details about how to care for your dental crown, let’s start by discussing what a crown is, how it’s created, and how it protects your tooth.
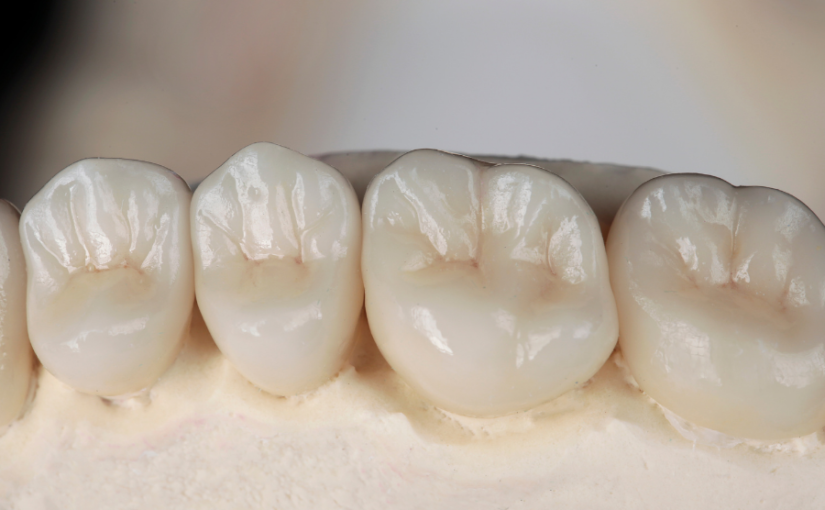
Although they can be fashioned from ceramic, metal, or a combination of the two, porcelain is the most popular and arguably the most effective material dentists use for crowns today. Porcelain is durable, feels the most natural, and is easily matched to the shade of your other teeth. Dr. Elizabeth Eggert and Dr. Jeff Eggert agree that all-porcelain crowns are the best overall choice nearly all of the time.
After Dr. Elizabeth Eggert or Dr. Jeff Eggert removes any tooth decay and reshapes your tooth, they will take a digital image or putty impression. In most cases, your crown can be created the same day at our office using the CEREC scan. Occasionally, we will need to send your impression to a dental lab, for the fabrication of your crown and you will return to our office in a couple of weeks for the placement. In this case, you’ll leave your first visit with a temporary crown and instructions for proper care.
Think about your dental crown as a protective helmet for your tooth. It fits intimately on top of your compromised tooth and is securely cemented in place. It looks and acts just like a natural tooth.
In addition to supporting weak or decaying teeth, crowns:
- Help hold dental bridges in place
- Cover severely stained or discolored teeth
- Protect a tooth after root canal treatment is completed to keep the tooth from splitting
- Are part of the system to restore a dental implant when you’re missing a tooth
With proper care, your crown should last a decade or more!
How can I take care of my dental crown to ensure crown longevity?
We’ve already established that crowns are highly durable and, among other things, help strengthen weak teeth. But although they’re durable, they’re not indestructible. Here are some important steps you can take to get the most life out of your dental crown:
1. Keep up with daily dental care.
The importance of daily brushing and flossing cannot be underestimated. Plaque can still form on crowns! Brushing and flossing twice daily helps remove sticky plaque before it builds up and keeps your teeth looking their best. It also removes food particles that get trapped between the crown and the gumline, causing plaque build-up that leads to gingivitis or decay and can aid in crown longevity.
2. Avoid chewy, sticky, hard foods.
Do you like to crunch on ice or chew hard candies? Just like natural teeth, crowns can crack under extreme pressure. Even healthy foods like popcorn with kernels and pistachios in the shell can cause undue damage to your dental crown. Taffies, caramel apples, and other sticky foods can loosen your crown, making it easy for food particles to get underneath and cause decay. In some instances, chewy foods can dislodge crowns completely. If this happens, call our office right away!
3. Minimize acidic and sugary foods.
Acidic and sugary foods will erode enamel, but even if your tooth is protected with the porcelain of a dental crown, these substances can still easily cause decay and damage the tooth under your crown.
If you choose to indulge in these foods, make sure you are using impeccable dental hygiene at home and it is super important that you maintain a regular recare schedule with us at Eggert Family Dentistry so we can discover any compromise early and before major damage occurs..
On a side note, acidic and sugary foods will cause enamel to wear thin, resulting in tooth discoloration and darkening. Because your dental crown is color-matched to your natural teeth at the time of application, discoloration of your natural teeth will create a contrast between those and your crown and detract from its natural appearance.
4. Wear a night guard if you’re prone to teeth-grinding.
Teeth grinding, also known as bruxism, is detrimental to your teeth in several ways. In addition to headaches and a sore, tired jaw, bruxism can wear down enamel and even cause teeth to crack or chip. Although molars can withstand 200 lbs of pressure from regular biting and chewing, they have their limit and so do dental crowns. Fortunately, wearing a night guard can protect your natural teeth and promote crown longevity. If you think you may need a night guard, talk with Dr. Jeff Eggert or Dr. Elizabeth Eggert about that at your next recare visit.
5. Prioritize your recare visits at Eggert Family Dentistry.
Your oral health is our first priority. In addition to a tooth cleaning by our magnificent hygienists, Dr. Elizabeth Eggert and Dr. Jeff Eggert will closely examine your teeth for any early signs of cavities, gum disease, and oral cancer. They will also perform annual x-rays, which can help spot early signs of infection and they will treat your teeth with fluoride to help remineralize them and prevent cavities. And, a recare visit wouldn’t be complete without a thorough inspection of any existing dental work, including dental crowns, to make sure they’re intact and functioning properly.
When it comes to oral health, prevention is always the best approach. If you haven’t been keeping up with your recare visits or have any dental concerns, Dr. Elizabeth Eggert and Dr. Jeff Eggert are happy to see you in our office. Call Eggert Family Dentistry at 651.482.8412 to schedule your next appointment.








![Do I Need a Dental Crown? [Answered]](https://blog.eggertfamilydentistry.com/wp-content/uploads/2023/11/Do-I-need-a-crown-answered-825x506.png)