By: Dr. Elizabeth Eggert
When you’re diagnosed with obstructive sleep apnea (OSA), your doctor may first prescribe CPAP therapy — you know, the face or nose mask attached to a machine that you have to wear at night. However, while CPAP therapy is extremely effective, many people can’t tolerate sleeping with it on every single night.
That’s why oral sleep appliances -– also known as mandibular advancement appliances — are also used to treat sleep apnea. In fact, they have an 80% compliance rate over the CPAP’s 40%.
We fit mandibular advancement appliances at Eggert Family Dentistry and have been able to help many people with OSA improve their sleep, oral health, and overall quality of life.
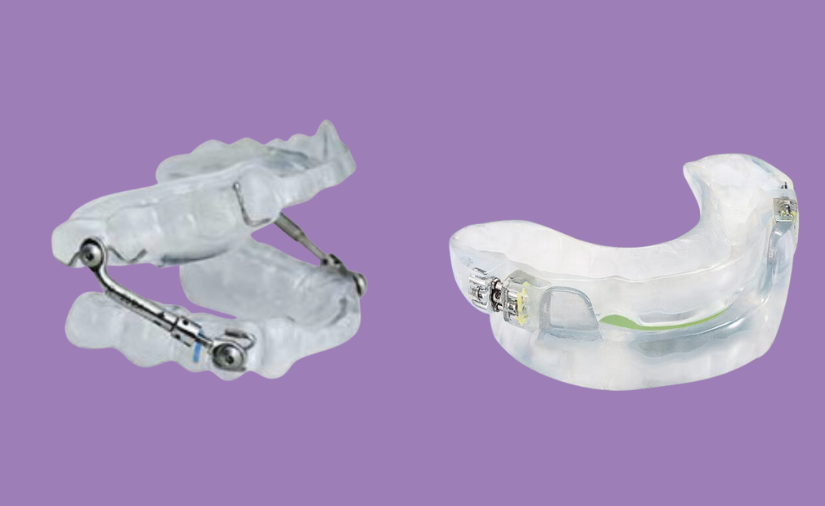
What is a Mandibular Advancement Appliance?
A mandibular advancement appliance (MAA) is a device that can be custom-fitted to a person’s mouth, and works by temporarily moving the jaw and tongue forward. This adjustment reduces throat constriction and opens up the airways, effectively preventing snoring and sleep apnea.
Benefits of Using a Mandibular Advancement Appliance
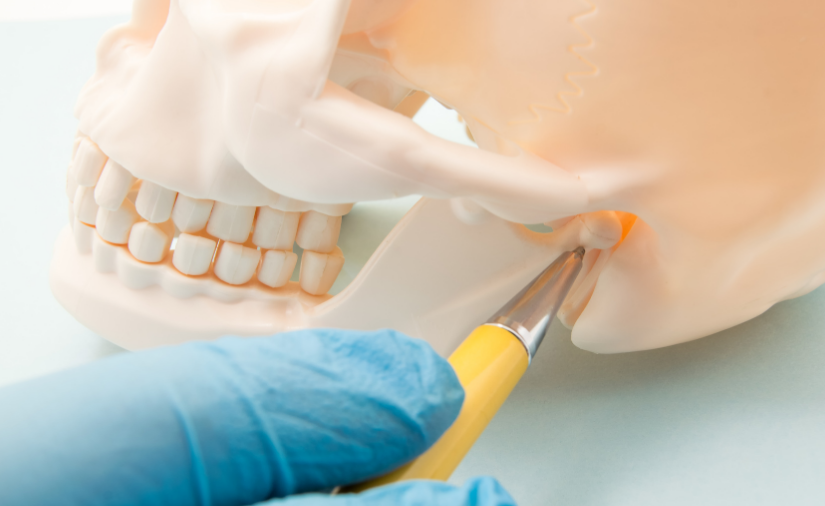
You probably already know that sleep apnea causes a myriad of health issues, most notably cardiovascular problems. But did you know that your sleep apnea also wreaks havoc on your dental health? People with sleep apnea also are more likely to experience TMD, bruxism, and dry mouth. Luckily MAAs can reduce and relieve each of these symptoms.
1. Relief from Tooth Grinding and Clenching
Many people who suffer from sleep-disordered breathing also grind their teeth or clench their jaw during sleep. This can lead to a host of dental problems, including tooth sensitivity, worn-down enamel, and even tooth fractures. MAAs can help alleviate these issues by positioning the lower jaw in a more forward position, which reduces the likelihood of grinding or clenching. The thought is that since the body can breathe better, the jaw doesn’t have to move around, trying to find the best position for air exchange.
2. Reducing Dry Mouth
People with OSA often sleep with their mouth open in an attempt to get more oxygen, which leads to dry mouth. Because saliva plays an important role in reducing the amount of plaque on your teeth, dry mouth can cause or accelerate tooth decay. Using an MAA will open up the airway and improve breathing, which will reduce the need to breathe through the mouth during sleep. This will reduce all dry mouth symptoms and keep tooth decay under better control by maintaining the proper amount of saliva in your mouth.
3. Reducing the Risk of Gum Disease
Gum disease is a common oral health problem that can lead to tooth loss if left untreated. People with sleep-disordered breathing are at an increased risk of developing gum disease, as the reduced oxygen flow to the gums can make them more susceptible to infection. By improving breathing and oxygen flow, MAAs can help reduce the risk of gum disease and promote overall oral health.
4. Improving Overall Sleep Quality and Quality of Life
Finally, the most important benefit of using an MAA is improved sleep quality, which can have a positive impact on your quality of life in general. Poor sleep quality has been linked to a range of health problems, and by improving breathing and reducing sleep disturbances, MAAs can help promote your overall health and wellbeing.
Want Better Sleep, Healthier Teeth, and a Higher Quality of Life?
If you have sleep apnea and would like to be fitted for a mandibular advancement appliance, Dr. Jeff Eggert or Dr. Elizabeth Eggert can help! After hearing from your medical doctor and doing an assessment of your bite, we can custom-design your device by taking impressions or digital scans of your mouth. Once the device is ready, we’ll ask you to come into our office for a fitting so we can make sure it’s comfortable and effective. Contact us or call us at 651-482-8412 today to schedule your mandibular advancement device consultation!








 When you come in for an appointment, we look for signs or symptoms that could be considered “red flags” for airway conditions, including sleep apnea. Dr. Elizabeth or Dr. Jeff perform an assessment to see if you have any of the following risk factors among many others:
When you come in for an appointment, we look for signs or symptoms that could be considered “red flags” for airway conditions, including sleep apnea. Dr. Elizabeth or Dr. Jeff perform an assessment to see if you have any of the following risk factors among many others: Did you know that, in
Did you know that, in  Bruxism is another condition that is often present alongside obstructive sleep apnea. Often intertwined with TMD, bruxism describes a condition caused by the clenching or grinding of teeth. It occurs unconsciously during sleep and can be another way a person’s body compensates for an airway obstruction.
Bruxism is another condition that is often present alongside obstructive sleep apnea. Often intertwined with TMD, bruxism describes a condition caused by the clenching or grinding of teeth. It occurs unconsciously during sleep and can be another way a person’s body compensates for an airway obstruction.