By: Dr. Elizabeth Eggert
With the school year in full swing, school sports have no doubt become an important aspect of many families’ lives. For all of us here at Eggert Family Dentistry, this time of year means we see an uptick in dental injuries and dental emergencies.
From football, to hockey, to baseball, dental injuries are extremely common for high school and middle school athletes. As a parent, it’s important to know how to deal with any dental emergencies in the event that a foul ball (or puck) causes an accident. Let’s take a look at the most common dental emergencies that arise out of school sports, and how to handle them.
The Most Common Dental Emergencies in School Sports
1. Tooth Fractures/Breaks: Chipped, cracked, or broken teeth are very common dental injuries experienced during impact sports. A direct blow to the face or a collision (whether it’s with equipment, a wall, the floor, or another person) can easily cause tooth fractures. While minor chipping on teeth doesn’t require immediate dental treatment, serious fractures can be painful and should be evaluated as soon as possible.
What To Do: Rinse out the mouth with water and hang onto those fractured pieces of tooth if possible. You can place the pieces of the tooth in water or milk to preserve them until you see us at Eggert Family Dentistry. Make an appointment as soon as possible to go over treatment options.
2. Avulsed (Knocked Out) Teeth: The same kind of impact that can cause tooth fractures and breaks can also cause a more serious problem: a knocked-out tooth. This is a very serious dental injury that requires immediate treatment.
What To Do: Hold the tooth by the crown (not the root) and rinse the whole tooth clean with water. If the tooth can be reinserted into the gum socket, do so. If not, put the tooth in a glass of water or milk to preserve the tooth until you can see Dr. Jeff Eggert or Dr. Elizabeth Eggert. Be sure to call our emergency line (Dr. Elizabeth’s cell number) right away and leave a detailed message. Call our office at 651-482-8412 to get the number for the emergency line.
3. Tooth Intrusion: Sometimes the problem isn’t that the tooth is knocked out of its place in the mouth, but that it’s pushed further into the gums and jawbone, which is called tooth intrusion. This kind of dental injury requires immediate dental attention to avoid any further complications.
What To Do: Don’t try to move the tooth on your own. Call Eggert Family Dentistry’s emergency line to make an emergency dental appointment as soon as you can, and in the meantime don’t chew at all (meaning no solid foods), or else you might make the intrusion worse.
4. Soft-Tissue Injuries: When your mouth is injured, it’s not just your teeth you have to worry about: your lips, cheeks, and tongue are at risk as well. Soft-tissue injuries include cuts, tears, or even puncture wounds that affect any part of your mouth apart from your teeth. These injuries can range from being mild and able to heal on their own, to serious and needing immediate attention.
What To Do: Clean the injured area by rinsing out the mouth with warm salt water. Apply a cold compress to minimize swelling and if the gums are cut, you can insert a cotton ball or cotton gauze to help the blood clot. If the bleeding doesn’t stop, call Eggert Family Dentistry for advice.
5. Jaw Fractures: Blunt force trauma to the face can result in a break or a fracture in the jawbone. This is a very serious injury that can be very painful, and requires immediate medical and dental attention.
What To Do: Using an elastic ACE bandage wrap or a large cloth (like a clean dish towel), secure the jaw lightly by wrapping around the top of the head and under the chin. Call Eggert Family Dentistry’s emergency line for advice, but likely you will need to be seen at Hennepin Country Medical Center, the local Level I trauma center and where they will always have an oral surgeon on call. Not all emergency rooms will be a good choice in this situation.
6. Orthodontic Emergencies: If a student athlete has any orthodontic gear in their mouth during a sports injury, such as braces, wires, or retainers, there may be broken wires or brackets that need to be fixed. While these issues usually don’t require immediate dental attention, they do need to be fixed as soon as possible in order to keep the teeth from shifting.
What To Do: Make an appointment with your orthodontist or Eggert Family Dentistry to have the orthodontic gear fixed as soon as you can. In the meantime, if there are any broken wires that are irritating the mouth, you can cover them with orthodontic wax.
7. TMJ Injuries: The temporomandibular joint (TMJ) can be injured as a result of a sports injury as well. This type of injury usually involves jaw stiffness, tightness, pain, or popping during movement. Depending on the amount of pain and difficulty of movement involved, this injury can range from mild to severe.
What To Do: Administer a cold compress to alleviate swelling and start taking an anti-inflammatory, over-the-counter medication, like ibuprofen. If things don’t seem back to normal after a couple of days, call for an appointment with Dr. Jeff Eggert or Dr. Elizabeth Eggert. It is helpful to examine the area of injury and determine how severe the injury is and what treatments are needed.
Preventative Measures to Help Avoid Dental Emergencies
As the saying goes, prevention is better than a cure! Or in this case, emergency treatment. Here are a few ways you can help your child prevent dental injuries from happening on game day.
Mouthguard: A mouthguard is one of the most effective ways to avoid a dental injury when playing sports. It is custom-fitted for your teeth and acts as a protective barrier, absorbing impact and preventing any major damage from occurring. Athletes should use mouthguards consistently during practices and games to safeguard their smiles.
Helmet/Face Shield: Depending on the type of sport being played, athletes may have the option to wear a helmet or face shield. In these cases, the athlete should always play it safe and wear their proper gear in order to protect their teeth (and the rest of their heads/bodies!).
Good Oral Hygiene: Which tooth is less likely to be knocked out or broken during a sports injury: a healthy tooth sitting in pink gums, or a decayed tooth sitting in gums that are inflamed or receding? If you guessed the healthy tooth, you’d be correct. One of the best ways to protect your or your child’s teeth is to make tomaintain proper oral hygiene habits to keep the teeth and gums healthy.
Recare Visits: A big part of keeping your teeth and gums healthy is staying on a regular schedule of recare visits with Eggert Family Dentistry, so we can monitor the health of your teeth and address any problems early on.
Dental Emergency? Contact Us!
If anyone in your family experiences a traumatic dental emergency, Eggert Family Dentistry is here to help! Call us immediately and schedule an emergency dental appointment with us. We’ll provide expedited professional care to your family to help repair any dental issues. In no time, you’ll be back on the field with a healthy smile! Call us today at 651.482.8412.



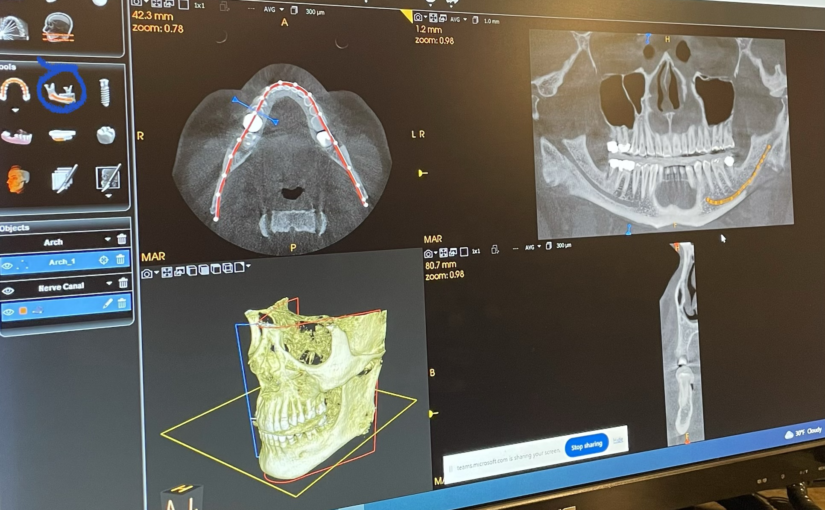
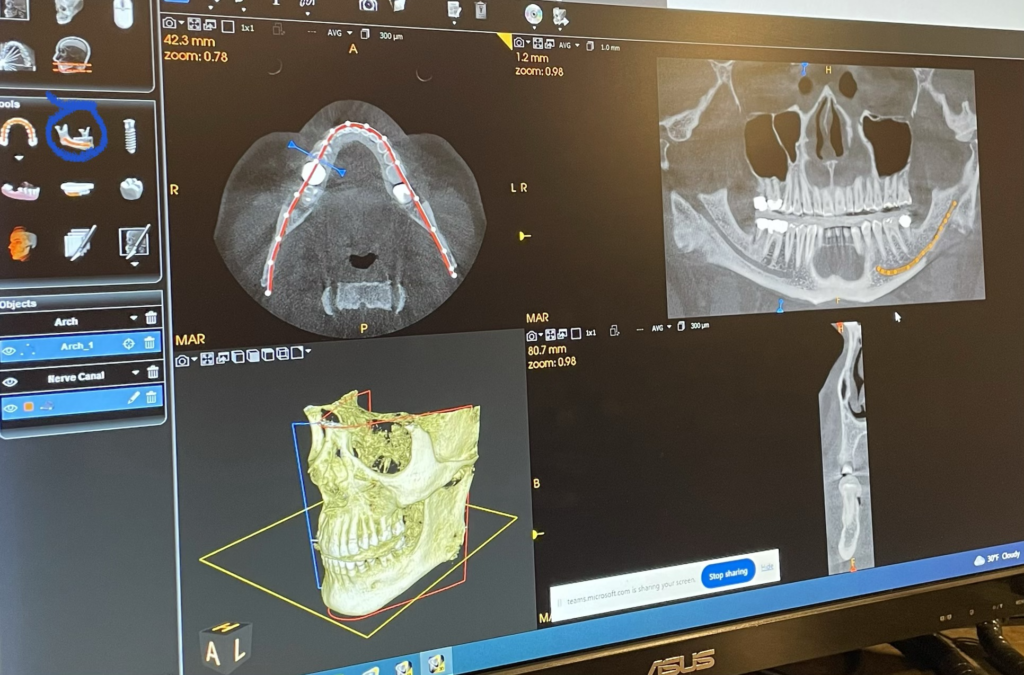
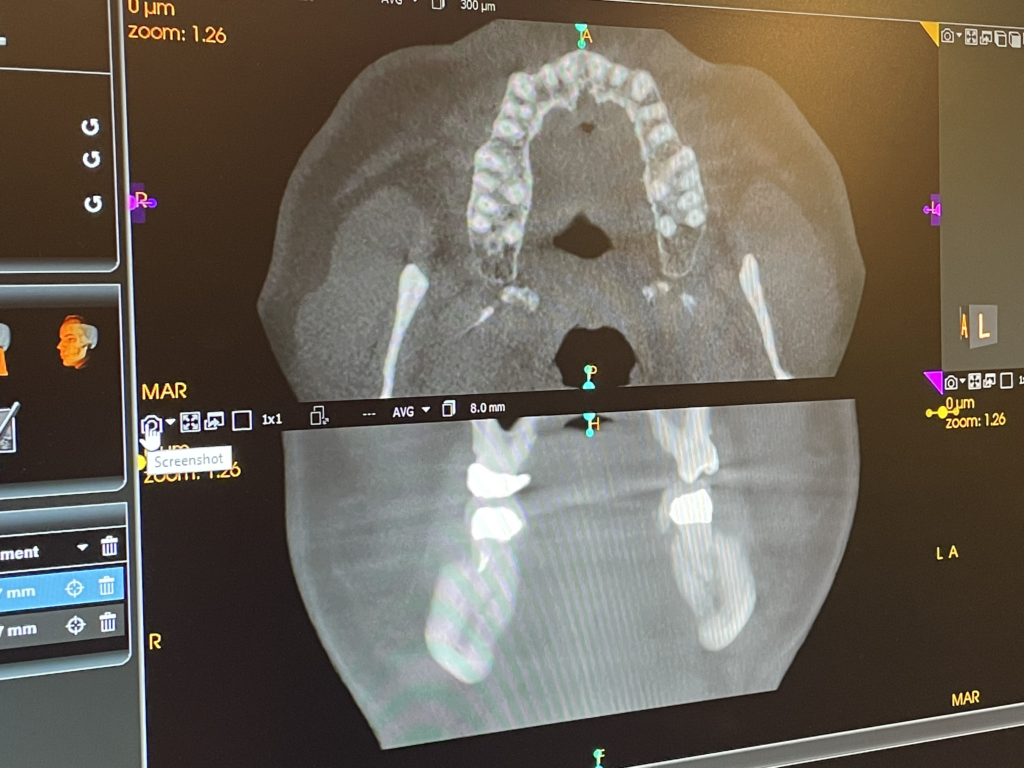
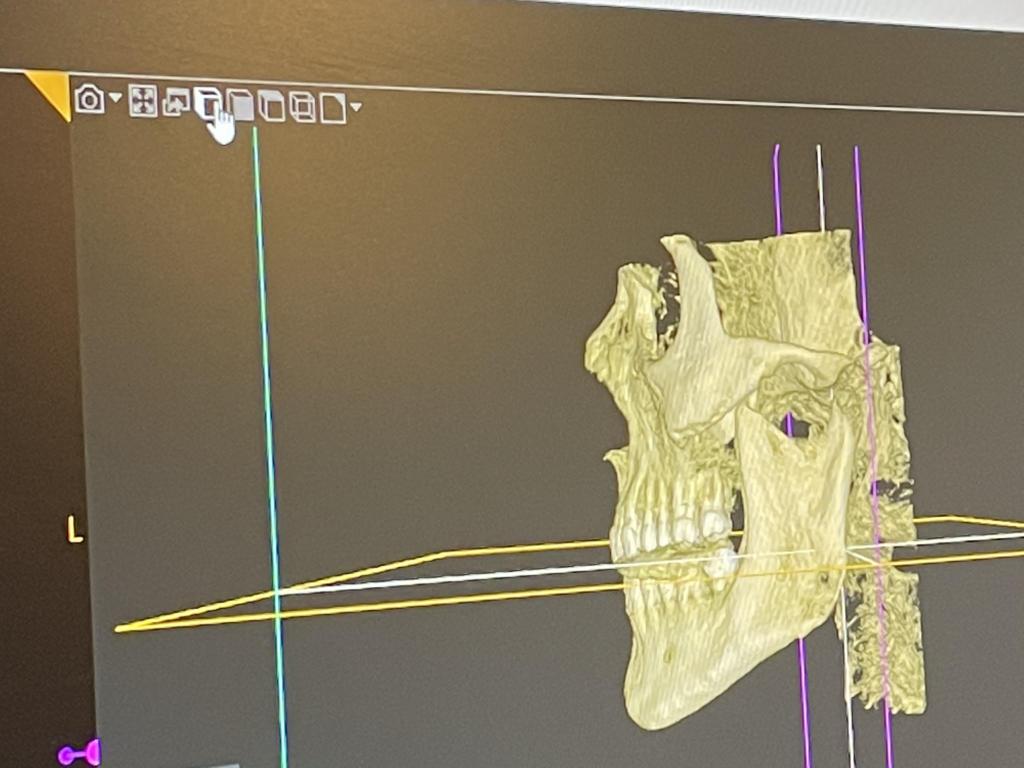
 One of the key features of the Carestream CS 9600 CBCT is its high image resolution, which allows for superior visualization of anatomical structures with minimal distortion. This level of clarity is invaluable in diagnosing complex dental conditions and planning precise treatment strategies tailored to each patient’s unique needs.
One of the key features of the Carestream CS 9600 CBCT is its high image resolution, which allows for superior visualization of anatomical structures with minimal distortion. This level of clarity is invaluable in diagnosing complex dental conditions and planning precise treatment strategies tailored to each patient’s unique needs. With this advanced technology at our disposal, we’re better equipped to evaluate and diagnose a wide range of dental issues, including infections, impacted teeth, jaw abnormalities, and even sinus problems. Additionally, the CBCT scan provides valuable insights into the TMJ, helping us identify signs of dysfunction and develop targeted treatment plans to alleviate discomfort and restore proper function.
With this advanced technology at our disposal, we’re better equipped to evaluate and diagnose a wide range of dental issues, including infections, impacted teeth, jaw abnormalities, and even sinus problems. Additionally, the CBCT scan provides valuable insights into the TMJ, helping us identify signs of dysfunction and develop targeted treatment plans to alleviate discomfort and restore proper function. As part of our commitment to providing exceptional care, we’re pleased to offer CBCT scans to all patients undergoing our Records Process in 2024 at no additional charge (a $435 value!). By integrating CBCT technology into our practice, we aim to elevate the standard of care and ensure that each patient receives the most accurate diagnosis and effective treatment possible.
As part of our commitment to providing exceptional care, we’re pleased to offer CBCT scans to all patients undergoing our Records Process in 2024 at no additional charge (a $435 value!). By integrating CBCT technology into our practice, we aim to elevate the standard of care and ensure that each patient receives the most accurate diagnosis and effective treatment possible.